This leaflet aims to help you and your family understand more about your radiotherapy treatment.
It will be given to you in addition to the information you will receive from your Clinical Oncologist (who is a specialist doctor in cancer treatment). Their team will be caring for you during your treatment. This team will include therapeutic radiographers and clinical nurse specialists but may also include other specialist health care professionals.
The leaflet describes radiotherapy planning and treatment. It also explains the side-effects which you may experience during and after treatment.
Each person’s treatment will vary, so the information given is a general guide. The healthcare team looking after you will explain your treatment and the side-effects in detail. If you have any questions after reading this leaflet, please speak to the team looking after you or ring the numbers at the end of the leaflet. Staff will make every effort to meet your individual needs or will direct you to the person who can help.
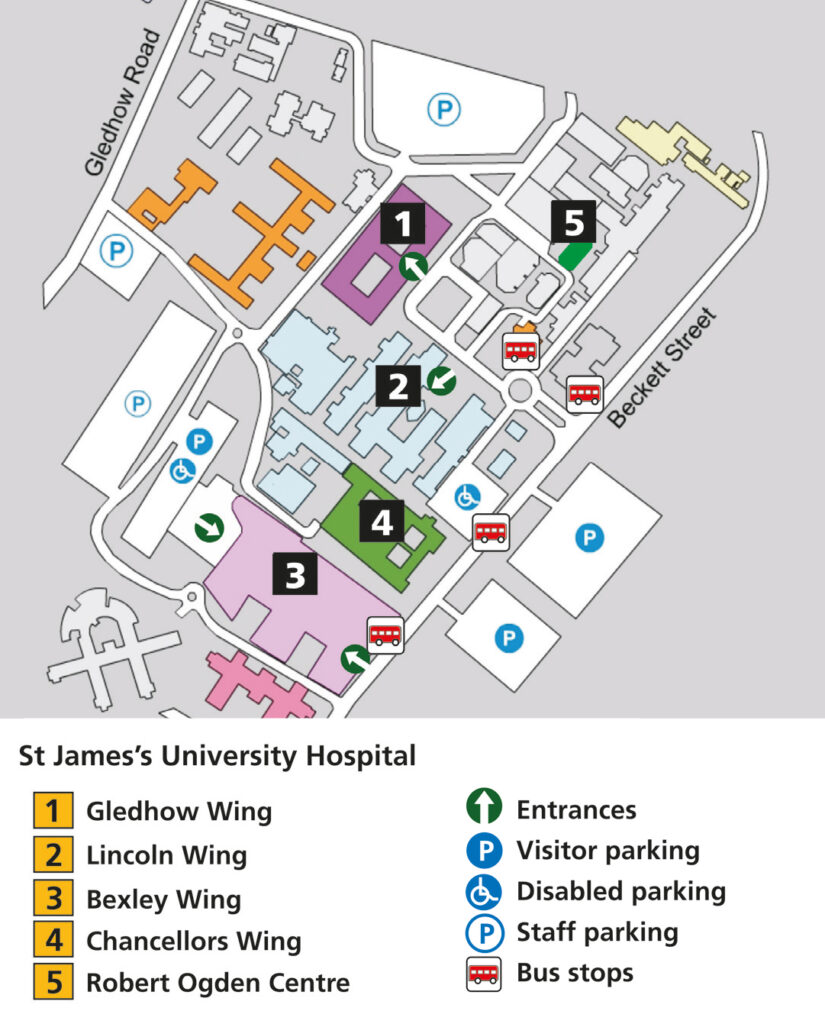
All your radiotherapy planning and treatment will take place in the Radiotherapy Department on Level -2, Bexley Wing, Leeds Cancer Centre (LS9 7TF).
Please note
Please do not bring any valuables into hospital with you as the Trust cannot accept liability for loss or theft.
What is radiotherapy?
Radiotherapy is the use of high energy x-rays and other types of radiation to treat cancer. The radiotherapy causes damage to cancer cells in the treated area. Although normal cells are also affected, they can repair themselves and are able to recover. Radiotherapy is a local treatment. This means it only affects the part of the body that is treated.
When you are having your radiotherapy you do not feel anything and it does not make you radioactive. You may hear a buzzing noise when the machine is switched on.
It is perfectly safe for you to be around others, including children and anyone who may be pregnant, throughout your treatment.
You will have your radiotherapy on a treatment machine called a linear accelerator, as shown here in the photograph. You will see your radiographers at each treatment session, and they will be happy to answer any questions you may have.
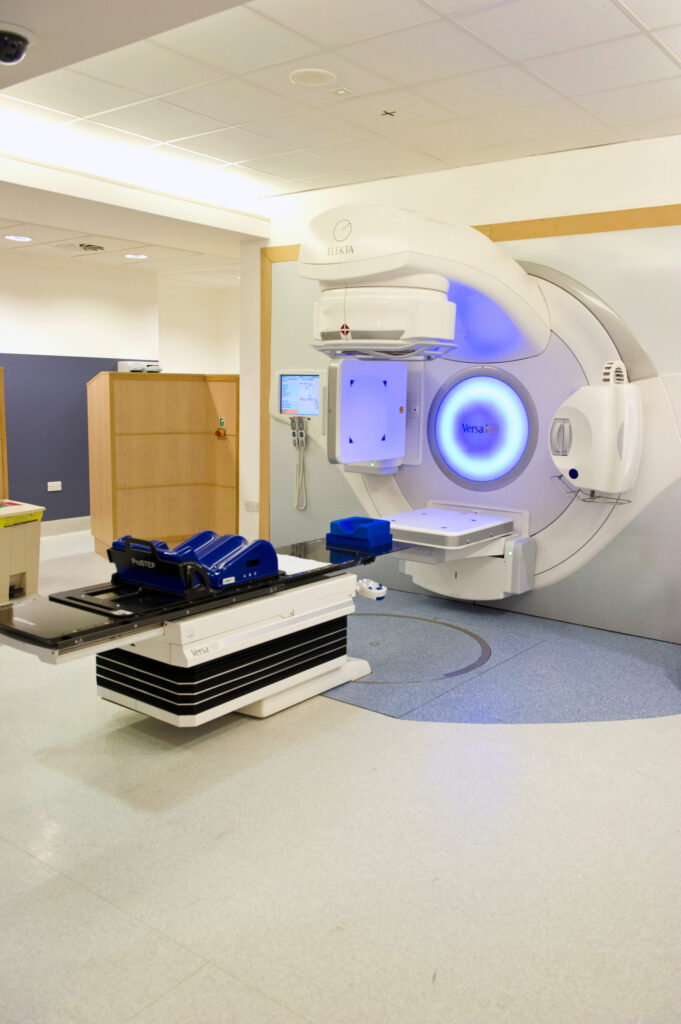
Photograph of linear accelerator in treatment room.
How often is it given?
Radiotherapy appointments usually last between 10 and 20 minutes. The treatment course is usually given over 1 – 35 treatment days. Treatment is usually given daily, Monday to Friday, however your treatment may not necessarily start on a Monday.
Occasionally you may need to be treated on a Saturday or Sunday due to a bank holiday. We will let you know if this is the case. Your radiographer will be able to explain the details of your individual radiotherapy appointments
Your treatment will usually be given as an outpatient.
Visiting us before your treatment
If you would like to visit the radiotherapy department before starting treatment, please call 0113 206 7603. This visit can be very useful as you can find out more information about radiotherapy and ask questions.
Patient quote:
“I was so pleased to see the machines before my treatment and the staff were so helpful and really put my mind at rest.”
Who will I meet?
Therapeutic radiographers
Radiotherapy is given by therapeutic radiographers of any gender. They are highly trained in the accurate planning and delivery of radiotherapy treatment.
You will see your radiographers at each treatment session and they will be happy to answer any questions you may have.
Student radiographers
The radiotherapy department is a training centre for therapeutic radiographers. They are supervised at all times. If you do not wish students to be present, please speak to a member of staff. This will not affect your treatment or care.
Others involved in your care
You may meet other staff whilst you are coming for radiotherapy. Everyone you meet will introduce themselves, tell you their job title and explain the role they have in your care.
Important advice before your treatment
Pregnancy
It is very important that patients who could become pregnant, are not pregnant at the start of their radiotherapy course. Also, patients should not become pregnant during their radiotherapy treatment, as this can have an effect on the unborn child. Use an effective form of contraception, for example condoms, coil, depo injection or contraceptive pill.
For more information see the ‘Contraception and pregnancy during cancer treatment’ (LN003721) leaflet.
Please do not hesitate to ask your doctor or nurse if you have any questions or concerns about these issues.
Planning your treatment
Your first appointment for radiotherapy will be a planning appointment. This will be used to gather all the information we need to accurately plan your treatment. We will contact you by phone, with an appointment for your radiotherapy planning session. Directions to the hospital and transport arrangements will be discussed with you at this point.
Some tests and scans may be needed to help plan your treatment. We will explain which of these you will need when your appointment is made. You may see your clinical oncologist (or a member of their team) at this appointment. This is an ideal opportunity for you to ask questions. If you have not previously consented to your treatment you will be asked to sign a consent form.
What to bring with you
- A list of all questions you may have.
- An up-to-date list of all the medications you are taking (including inhalers, sprays, vitamins or herbal products).
- Any medication that you may need during your visit.
- Something to eat and drink and something to occupy yourself with as this first visit can be quite lengthy (up to two hours).
Mould Room (if you need a radiotherapy mask)
Radiotherapy involves exact positioning of the radiation beam, so you will need to stay very still while you are having treatment. To help you stay still when treating the head, neck, upper chest or armpit areas, we make a mask for your head and shoulders. You will wear your mask for your planning scan and treatments.
You will be given an appointment to attend the Mould Room where the masks are made.
If you have any concerns about the mask, please let your clinical oncologist or a member of their team know. They will help you or contact the support team who will be able to help you.
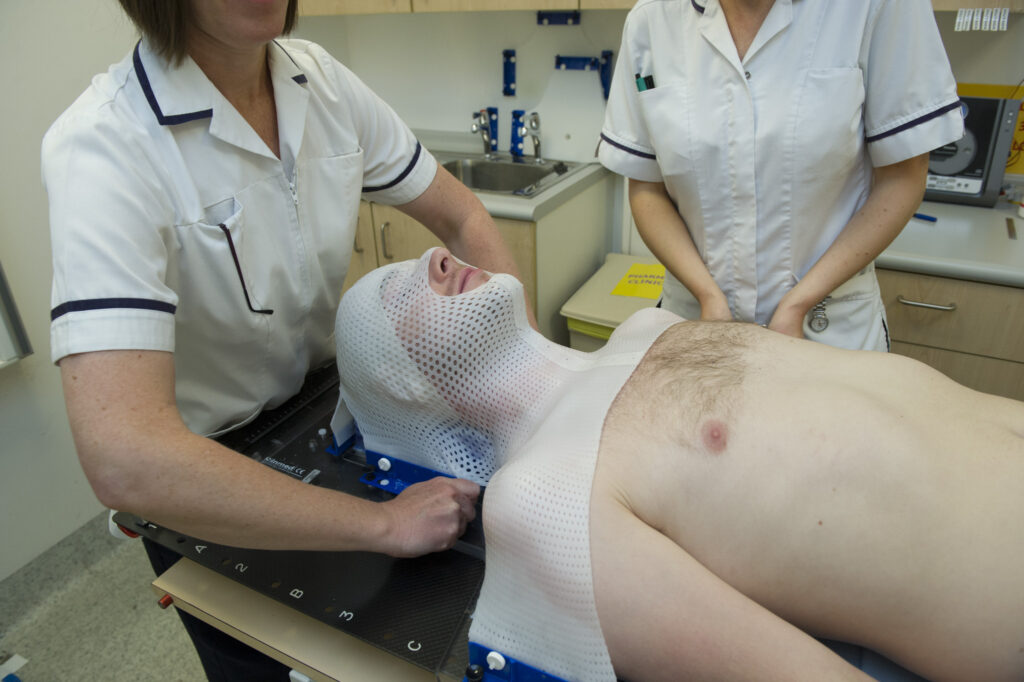
There is a leaflet called ‘Having a radiotherapy mask made’ (LN000001) available with more information about masks.
Your planning scans
In order to plan your radiotherapy treatment you will need a CT scan, or an MRI scan, or both.
Your CT planning scan
The planning CT scan is done on a machine called a CT scanner, as shown here in the photograph.
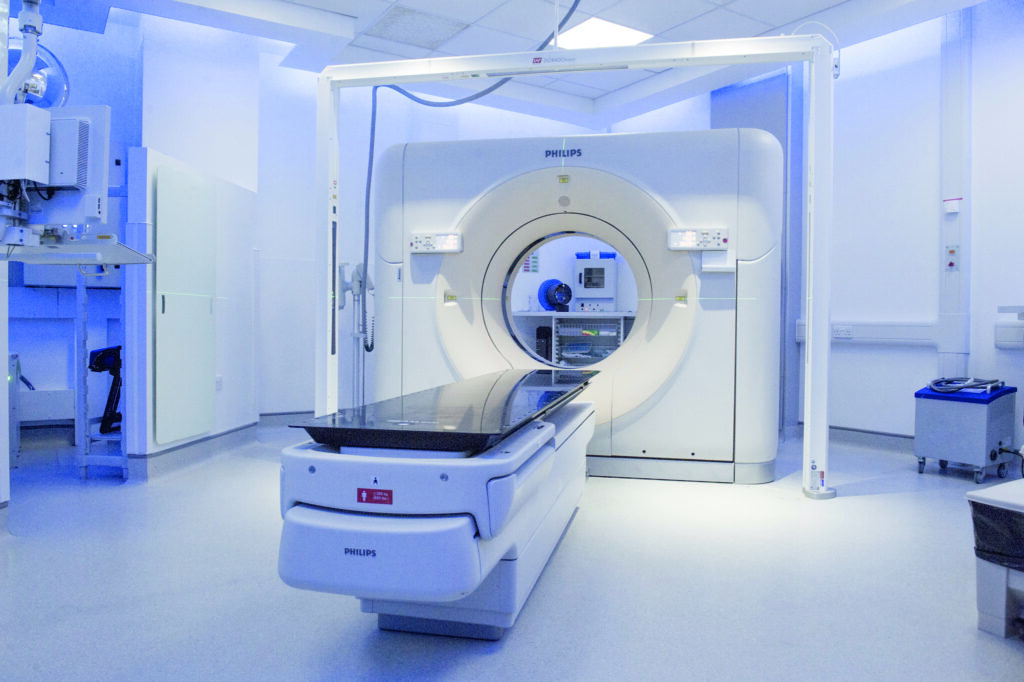
It allows the images from the scan to be sent to the radiotherapy computer planning system. There will be several members of staff present at your scan. These will include therapeutic radiographers, and possibly a mould room technician and a dosimetrist (the person who will produce the computer plan for your treatment). The radiographers may draw some marks on your skin, to be used as a reference.
Planning scans are not diagnostic examinations and will not be reported on as such.
You will then be scanned. This should only take a few minutes. At the end of the scan any skin marks may be replaced by a small permanent mark (tattoo). These permanent marks help to ensure that you are in the same position each day. It also means that you can wash without worrying about your marks coming off. Please note: Not all radiotherapy patients will need these permanent marks. Please ask your radiographer if you want clarification.

Following the planning scan(s) the radiographers will give you the time of your first appointment on the treatment machine. This is most likely to be a couple of weeks after the planning visit. The radiographers will talk to you about any further appointments you have.
Contrast (dye)
A special contrast agent, often called a dye, may be used for your scans (CT and / or MRI) to make specific organs, blood vessels and/or tissue types appear clearer in the scan images. This can make it easier for the Oncologist to plan your treatment. The dye is given through a very small plastic tube called a ‘cannula’ into a vein in your arm. You should tell the radiographer if you have any allergies, but they will go over this before they use any dye.
The radiographers will advise you about drinking plenty of fluid after your injection.
Contrast side-effects
You may notice a warm feeling throughout your body and have a metallic taste in your mouth. You may also feel as if you have passed urine. This will pass very quickly. There is a slight risk of an allergic reaction to the injection, such as a skin rash, but this very rarely may lead to other complications.
The staff in the radiotherapy department are highly trained to manage any complications and again the risk involved is very small. You will be able to drive your car or go to work after your scan.
Your MRI planning scan
Some (but not all) patients may need an MRI planning scan in addition to their CT Planning scan. Other patients may only need an MRI planning scan, and not a CT planning scan. If you are having both, the MRI planning scan usually takes place on a different day to your CT scan. Before you enter the MRI scanner room we need to make sure it is safe for you. This is because the MRI scanner contains a large magnet. You will need to remove any items that contain metal for the scan. You will lie in the same position that you will have your treatment in. We will give you some earplugs and headphones to wear as the scanner can be quite noisy. The MRI scan can take up to an hour.
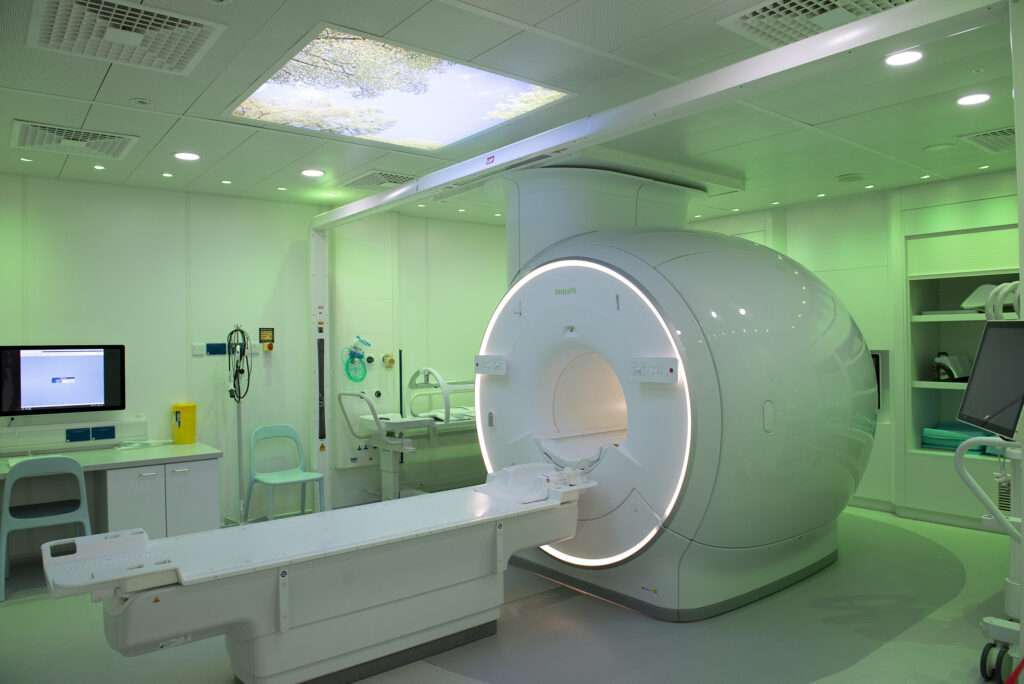
This MRI planning scan is not a diagnostic scan and will not be reported on.
We will contact you by phone, with appointments for these sessions.
Having your treatment
When you arrive for your treatment you should go to the radiotherapy main reception desk at the entrance of the radiotherapy department. On the first occasion you will be given a list of all your appointments and be escorted to the waiting area for your machine.

The radiographers will explain what will happen and answer any questions that you may have.
As previously stated, treatment is usually given Monday to Friday, however your treatment may start on any day of the week. Whenever possible you will be treated at the time of day that suits you, but this cannot always be arranged or guaranteed. There may be occasions when you may have a longer stay in the department or be asked to attend at a different time, for example to see your clinical oncologist.
You may need to undress and put on a gown; the radiographers discuss this with you when you first attend the department.
The radiographers will position you, and adjust the treatment couch and machine to the correct positions. For the first few treatments and also intermittently during treatment the radiographers will take images to check the accuracy of the treatment. This will take a few more minutes.
Please note
These images do not monitor your condition but are purely for treatment accuracy.
You will be asked to stay as still as possible during the treatment but you should breathe and swallow normally. Once you are in the correct position the radiographers will leave the room to switch on the machine. You will only be alone for a few moments at a time.
The radiographers will be watching you on a closed circuit TV (CCTV) monitor during treatment.
The CCTV camera is not recording or saving any images. There is also an intercom system so the radiographers can talk to you.
If you would like to listen to music during your treatment, please let us know. The treatment only takes a few minutes but you will be in the treatment room for about 10-20 minutes.
The machine stops automatically after your prescribed dose of treatment has been given. The radiographers can stop the machine at any time if needed. The treatment machine makes a buzzing sound when switched on. You do not feel anything.
The radiographers may need to come in and out part way through each treatment.
After the treatment is complete the radiographers will come back into the room and help you off the couch.
Your treatments will generally be on the same machine. However, there may be days when this machine is being serviced and your treatment will be in a different room.
On some days the radiotherapy department may be busy and there may be a delay before your treatment. We will keep you informed of any delays over 30 minutes. Please see the delay boards in the waiting areas. It may be a good idea to bring something to eat and drink with you, including any supplement drinks you have been asked to have and any medication you may need.
Important
It is very important that you do not miss treatment days as it may make your treatment less effective. If you feel you are unable to attend for any reason please telephone us so that we can discuss this with you. If you have any queries about your appointment times please discuss these with the radiotherapy coordinators on your treatment unit. For appointment queries please telephone the radiotherapy reception desk 0113 206 8940 for further advice.
Please ask your GP for further prescriptions for on-going medication after finishing your treatment.

Research at Leeds Cancer Centre
Leeds Cancer Centre is a major centre for cancer research. You may be asked if you would like to help with some of the clinical studies. You are under no obligation to take part in any trials, and your treatment will not be affected in any way if you do not wish to take part.
If you do take part in a clinical trial you may meet a research nurse or radiographer who will be helping to run the trial.
Side-effects
Side-effects can be divided into short term (acute) effects that happen during or soon after treatment, and long term effects occurring months or years later. Some side-effects are common, whilst others are rare. The area and amount of treatment given to you will affect which side-effects are most likely to happen to you. Your clinical oncologist will discuss this with you. If you develop any radiotherapy side-effects you will be given advice and support by your healthcare team.
Short term side-effects from radiotherapy
Most side-effects are common and are temporary. Side-effects tend to build up from about the second week of treatment and will be at their worst at the end or just after the treatment course. They generally last a number of weeks or months after the treatment has finished.
Skin reaction
The skin in the treated area may start to redden or darken around 10 days after starting your radiotherapy. It may become dry and itchy. For a very small number of patients, it may peel and become weepy. Avoid hair removal where possible, including shaving, waxing, cream and lasers unless advised otherwise by your consultant, nurse or radiographer.
Before you start your treatment, a radiographer will explain what could happen to your skin and how to look after it. They will also give you a leaflet to take home.
Tiredness (fatigue)
Nearly all patients having radiotherapy will feel tired. Be prepared to take things easy during treatment and allow for extra rests. Try to continue with some of your normal routines and activities if possible.
Fatigue usually improves in the weeks to months after treatment.
Things you can do to help include:
- Gentle exercise can help reduce the symptoms of fatigue.
- Having enough to drink can prevent tiredness from dehydration.
- Small meals or snacks eaten more often than three times a day may be easier to face.
- Try to get a good night’s sleep where possible, a daytime nap may help.
- Try to ‘pace’ yourself, listen to what your body is telling you, rest if you need to.
- Pick out the things that you enjoy, and try to accept help for some tasks.
- Little and often is the rule of thumb.
There is a Macmillan information leaflet available called ‘Coping with fatigue’. If you would like a copy or support with your fatigue, please ask a member of staff.
Loss of appetite
Your appetite may vary during your treatment. Try to eat well during your treatment and also drink about two litres of fluid each day. There is a leaflet called ‘Eating well during your treatment’ (LN000031). Please ask a member of staff if you would like a copy or follow the link below:
Hair loss
Only hair in the treated area will stop growing and may fall out. Your doctor will tell you if you might lose your hair.
Sometimes hair will not grow back after treatment.
Possible long term side-effects from radiotherapy
Long term side-effects will depend on the exact details of your treatment.
If you are concerned about your risk of developing any of the following side-effects please speak to your consultant or specialist nurse.
Cancers caused by the radiotherapy
When you have had radiotherapy there is a small risk that cancer can develop many years later, however this is rare. If you have any concerns, please discuss this with your consultant.
When radiotherapy has finished
Your side-effects may get worse in the first few weeks after treatment and will then gradually settle. You should start getting back to normal about 4-6 weeks after treatment but it may take a little longer. Tiredness can last for several months and you may need to continue to rest more than usual.
You may be asked to attend the hospital where you were first seen by your oncologist for follow-up checks at regular intervals. This will vary according to the area you have had treated. Please discuss this with your doctor if you have any concerns.
Planning a return to work
If you find that you are tired after your treatment has ended you may consider taking a break from work or working part-time. It can be useful to talk to your employer about returning to work gradually, i.e. shorter or fewer days at first.
Your GP can recommend this on your fitness to work note. The Macmillan booklet ‘Work and Cancer’, offers help and advice on all areas of work during your cancer treatment.
Vaccinations or flu jabs
Please ask your consultant for the latest advice on having vaccinations or flu jabs.
Leisure or physical activities
Whatever physical activities you wish to take part in, remember to start slowly and build up the amount of exercise gradually.
Further information and support
If you have any questions please ask your hospital team. We all have our own ways of coping with difficulties.
Some people have a close network of family and friends who provide emotional support. Others would rather seek help from people who are not involved with their illness.
The following are also available as sources of information and support that you may wish to use.
Clinical Nurse Specialists (CNS)
Your CNS is available to discuss any aspect of your treatment with you. You will be seen by a CNS before your treatment. This is to offer support and advice about the practicalities and effects of your treatment and answer any questions you may want to ask.
Your CNS will also assess and discuss any physical, psychological, social, occupational and spiritual needs that you may have.
They can refer you to other services if needed, for instance, benefits advice. You should be given a ‘key worker’ as a contact for support through your treatment; this is usually your CNS.
Macmillan Specialist Radiographer and Macmillan Radiotherapy Nurse Specialist
Sometimes people need more help if they are feeling depressed, very anxious or are having problems with their treatment. If this is the case you may benefit from seeing the Macmillan radiographer or nurse specialist.
Your clinical oncologist, radiographer or nurse can refer you at any point before or during your treatment.
Benefits and financial help
All patients with cancer are able to receive free prescriptions. Ask for a FP92A claim form from your GP or the hospital.
Benefits can change. For up to date information please speak to your nurse specialist, or ask at the information centres in Bexley Wing or at the Maggie’s Centre.
Talking to children
You may need to talk to your children about your treatment and may not know where to begin. Talk to your doctor or visit the Information Lounge for written information.
Macmillan Cancer Support have produced a booklet, which will help you explain what cancer is and how it may be treated.
Local Support Services
Leeds Cancer Support
Leeds Cancer Support complements care provided by your clinical team. We offer access to information and a wide range of support, in a welcoming environment for you, your family and friends.
We can be found in the information lounges in Bexley Wing and also in the purpose built Sir Robert Ogden Macmillan Centre (behind the Thackray Medical Museum).
The Sir Robert Ogden Macmillan Centre
The Centre is on the St James’s Hospital site and offers a variety of support services including complementary and supportive therapies.
Contact numbers for Leeds Cancer Support
Maggie’s Centre
If you or someone you love has cancer you may have lots of questions. Maggie’s is a warm, welcoming place where you can meet people who are experiencing similar things to you.
You may also be able to find support groups specific to your needs and get advice and information from their professional staff.
You don’t need an appointment and all support is free.
Useful organisations
Car Parking
When you are coming for radiotherapy planning and treatment your parking is free in the on-site multi-storey car park. Please ask for more information at the radiotherapy main reception desk.
Refreshments
There is a restaurant and coffee shop available on Level 0, which are open daily. They serve drinks, light snacks and hot meals. Vending machines are also available in the main radiotherapy waiting room and Level 0.
There is also a shop on Level 0 with books, papers and snacks.
Hotel Bexley Wing
Patients having radiotherapy or chemotherapy sometimes use the hotel if they have a long way to travel. The hotel is located on the 8th floor of Bexley Wing and offers 19 twin rooms and 1 single room. All have en-suite, tea and coffee making facilities, a mini fridge, towels, hairdryer and digital television. There are two rooms with wheel chair access and a wet room. Patients are able to stay free of charge. There is a charge for relatives if they are staying in their own room.
Meals can be purchased (at breakfast and lunch) if you are able to make your way to the restaurant in the Bexley atrium. At other times you will need to have something you have brought from home or purchased.
There is a very small fridge for your personal use. There are no staff after 4pm until the next morning in this facility.
How to find us
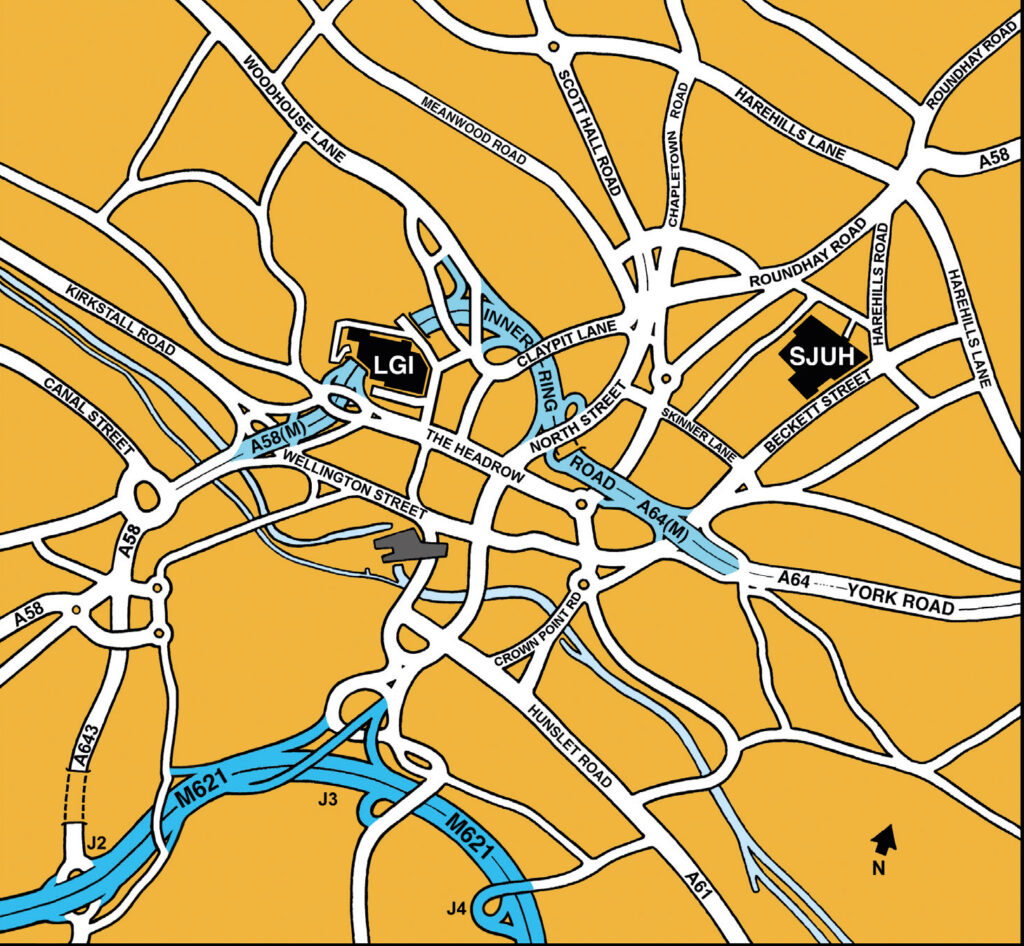
St James’s University Hospital – site plan