Your liver surgeon has recommended for you to have a Transjugular Intrahepatic
Porto-Systemic Shunt (TIPSS).
This leaflet will explain what this operation involves, the intended outcomes and the possible risks.
What is a transjugular intrahepatic porto-systemic shunt?
TIPSS or transjugular intrahepatic porto-systemic shunt is an operation that creates an internal ‘bypass’ between the ‘portal vein’ and the blood vessels draining blood from the liver back to the heart (the hepatic veins).
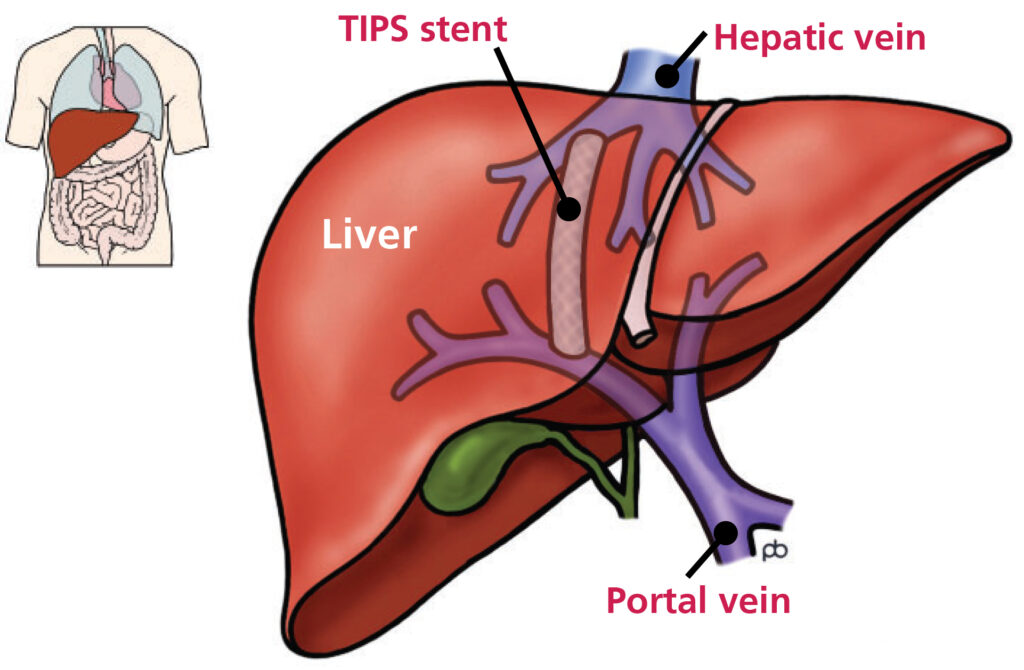
This reduces the pressure within the portal vein and allows for blood to flow more freely back to the heart, bypassing the scarred liver. TIPSS is performed to reduce complications of high blood pressure in the portal vein such as bleeding from varices (thin-walled veins that are distended and can rupture), and ascites, an uncomfortable distention of the abdomen resulting from fluid accumulation.
In rare occasion, a TIPSS may be recommended for patients with increased portal blood pressure, in patients with Budd Chiari Syndrome, or in patients who had a liver transplant.
How is a TIPSS performed?
Anaesthetic
An anaesthetist will look after you closely during a TIPSS operation as it is normally done under general anaesthetic. A small cannula is inserted in your arm that allows the anaesthetist to give you medicines to send you to sleep. Once asleep, the skin over the side of the neck is cleaned with an antiseptic.
Operation
During the operation, a small tube called a ‘catheter’ is inserted into a vein in the neck, via a tiny skin puncture. X-ray is used to guide the catheter into the hepatic vein in the liver. A needle is then used to create a track between the hepatic vein and portal vein through the liver tissues. Once the track has been made, it is enlarged using a balloon and the enlarged track is kept open by inserting a fabric tube with a metal supporting scaffold (known as a stentgraft). Whilst the balloon is taken out, the stentgraft is left permanently in the liver.
Consent
The anaesthetist will consult with you beforehand to discuss the general anaesthetic plan.
The operating interventional radiologist will explain the operation to you in more detail and answer any of your questions to your satisfaction before you provide your permission and sign your consent form.
What are the risks?
TIPSS is overall a safe operation. There is a 1-2% risk of major complications but in 98% of those treated develops no problems.
- Bleeding (6%) and infection (14.5%).
- The bypass effect of TIPSS may cause deterioration of liver function that could result in liver failure (in about 1% of patients, the liver does not recover, resulting in liver failure and imminent death).
- Confusion or hepatic encephalopathy may occur as the blood from the bowel bypasses the liver, leading to chemical changes in the circulation that can affect brain function (about 1 in 10 patients will show signs of confusion); this can be treated by altering diet and medications but in 1% of cases, these measures may not work.
- As TIPSS is performed under general anaesthetic, the anaesthetist will discuss the risks of this with you, prior to the operation.
- Allergic reaction to contrast dye (mild symptoms like nausea, itchiness / rashes about 3%; moderate – severe symptoms like severe vomiting, bronchospasm occur in > 1%; risk of death is rare, estimated at 1:170,000).
- X-rays will be used to make images of your body and guide your doctor during the procedure. X-rays are a type of radiation. We are all exposed to low levels of natural radiation as part of our everyday lives and medical x-rays give an extra dose of radiation. Radiation can increase your chances of developing cancer many years or decades after the exposure. The chances of this happening to you as a result of this procedure are considered to be low. In some very rare situations, you might experience some reddening of your skin in the area that was treated. If this happens, you should contact your clinical team who will be able to give some advice on the simple steps you can take to look after your skin. It is important to remember that your doctor thinks that the benefits of this procedure outweigh any risks from the radiation. We will make sure that the amount of radiation used in your procedure is as low as possible.
Are there alternative investigations / treatments?
There are open surgical operations available to achieve similar results, although these are comparatively riskier and more invasive than a TIPSS.
Some varices may be managed by injecting glue or using elastic bands inserted via a camera down the gullet into the stomach (endoscopy). Most patients will have had several treatments like this before being referred for a TIPSS.
If the bleeding cannot be controlled via endoscopy, an emergency TIPSS may be needed.
Ascites can be managed with medicine or with a procedure called paracentesis, which is either an intermittent or permanent drainage of fluid from the abdomen. Most patients with ascites will be on water tablets and/or regular paracentesis. Patients undergoing TIPSS have usually had these other treatments attempted with variable success.
What to expect from this operation?
Admission
You will be admitted the night before your operation under the care of the liver team or you may already be on a ward. Your doctor will arrange:
- Specific and up-to-date blood tests are required to make sure it’s safe to carry out the operation.
- A cannula will be inserted in your arm, and you may need a fluid drip overnight or antibiotics before your operation.
Pre-operative preparation
To promote patient safety during your operation, the following patient preparation are required:
- Fast for a minimum of six hours prior to your operation, although you may still drink clear fluids like water up to two hours beforehand.
- To lessen your risk of getting an infection, you will be prescribed a course of antiseptic wash and nasal cream.
- Most blood thinning medications need to be omitted, please discuss with us if you are taking any.
- If you have bleeding disorders or your blood clotting function is above threshold, you may require a blood transfusion; please inform us if you have concerns.
Recovery
TIPPS usually takes about 2-3 hours, though every patient is different, and some operations may take longer. Immediately after your operation:
- You will be transferred to the post-anaesthetic care unit (PACU), where you will be closely monitored.
- You will be placed on bed rest for several hours to allow you to recover from the anaesthetic drugs and reduce your bleeding risk.
Aftercare
Once stable, you will then be transferred back to the liver ward to recuperate. You may expect the following:
- TIPSS results in increased blood flow back to the heart that may cause shortness of breath in some patients, which can be treated with a course of water tablets.
- If the operation was performed to treat ascites, you may find that you pass increased amounts of urine for the first 24-48 hours. This suggests that the TIPSS is working; however, you may require a drip if you are unable to drink sufficiently.
- Your blood tests will also be checked to make sure the liver is working properly after the TIPSS after the first day or so, and your liver doctor will inform you when it’s safe for you to be discharged from the hospital.
Care at home
All being well, you will normally be discharged after 2-3 days.
- Exercise: limit your activities, get plenty of rest and gradually introduce light exercise after a week.
- Work: we advise a period of about 10-14 days off-work to rest after a TIPSS; a sick note may be requested from your liver doctor if needed.
- Driving/travel: no definite contraindication for traveling; however, you are advised not to drive for at least 72 hours after your operation.
- Medicines: your medications will be sorted by a ward doctor before you’re discharged; it is best to keep your usual pain medications at home, when required.
- Follow-up: a scan of the TIPSS will be arranged at 6 and 12 months after your operation; if you live away from Leeds, these can be done in your local hospital. Some follow-up scans may find narrowing of the TIPSS overtime, requiring a procedure to stretch the TIPSS with a balloon (about a 3/4 of patients with a TIPSS may require this procedure over the remainder of their lifetime).
Contact details
We hope some of your questions have been answered by this leaflet. If there are any questions you would like to ask before you come for your operation, please get in touch.
Via telephone:
Your GP or NHS direct on 111 (routine) or 999 (in an emergency)
Via email
How to get to our department
We are located in the Ground Floor of Lincoln Wing at St James’s University Hospital.
Follow the link for more information on how to find us