This leaflet has been given to you to help answer some of the questions you may have about a vaginal pessary. It explains what we use a pessary for (vaginal prolapse), the benefits, risks, and alternatives.
What is a vaginal prolapse?
Pelvic organ prolapse is a common condition where the walls of the vagina start to collapse and fall inwards (weakness of the pelvic floor). Half of people who have been through pregnancy and childbirth, may develop a prolapse, but not all will have symptoms, however, it is more common as you age.
Weakness of the pelvic floor can happen for a variety of reasons:
- Chronic constipation
- Persistent coughing
- Childbirth
- The natural ageing process
- Surgery
- Occupation
- Menopause
- Being Overweight
Types of prolapse
Pelvic organ prolapse occurs when the support of the pelvic organs begins to weaken. This may result in a number of different prolapses. When the front or back wall of the vagina prolapses, the organ behind it (the bladder or bowel) usually follows it down and adds to a bulge. The womb (uterus) can lose its support and descend into the vagina. The top of the vagina can also prolapse if you have had a hysterectomy, called a vault prolapse.
Examples of female anatomy with and without prolapse.
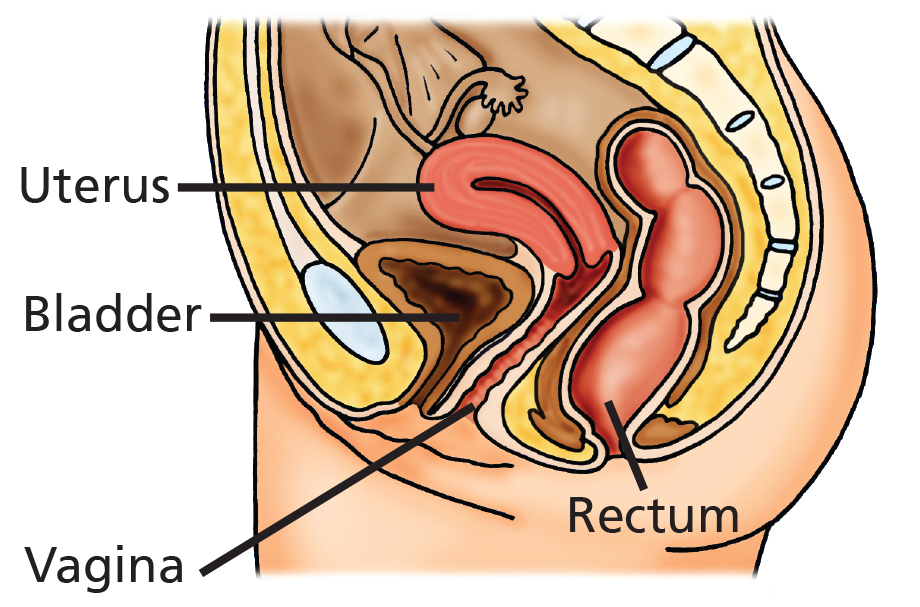
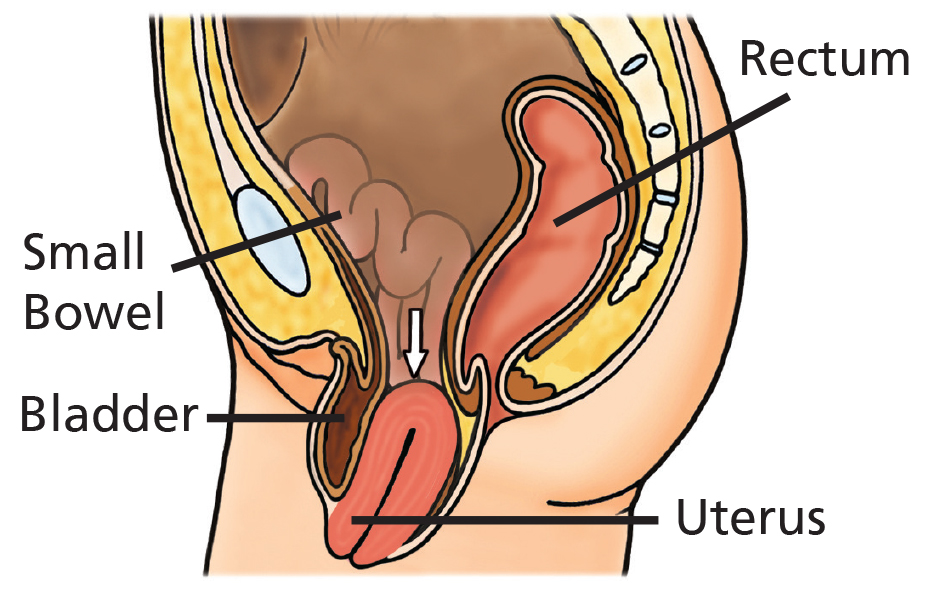
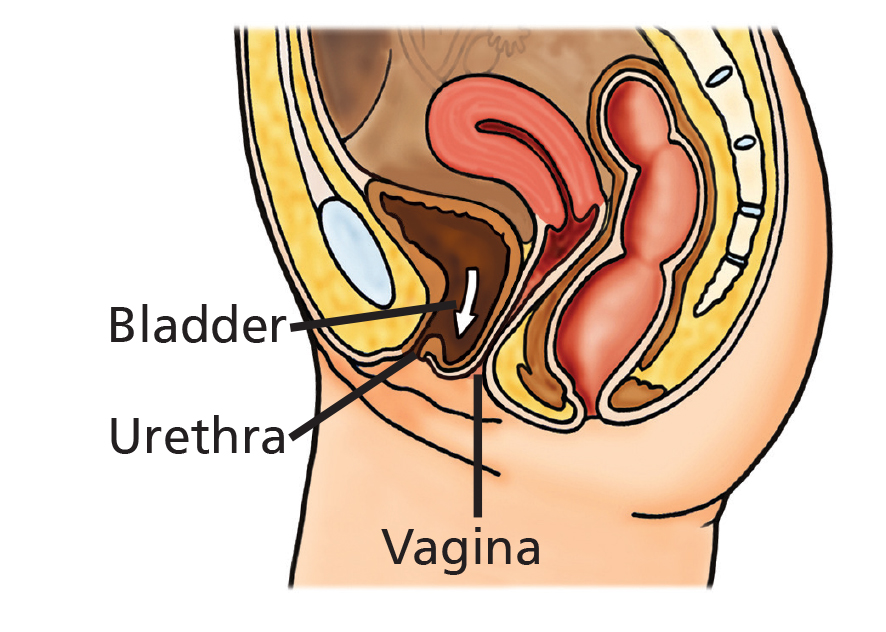
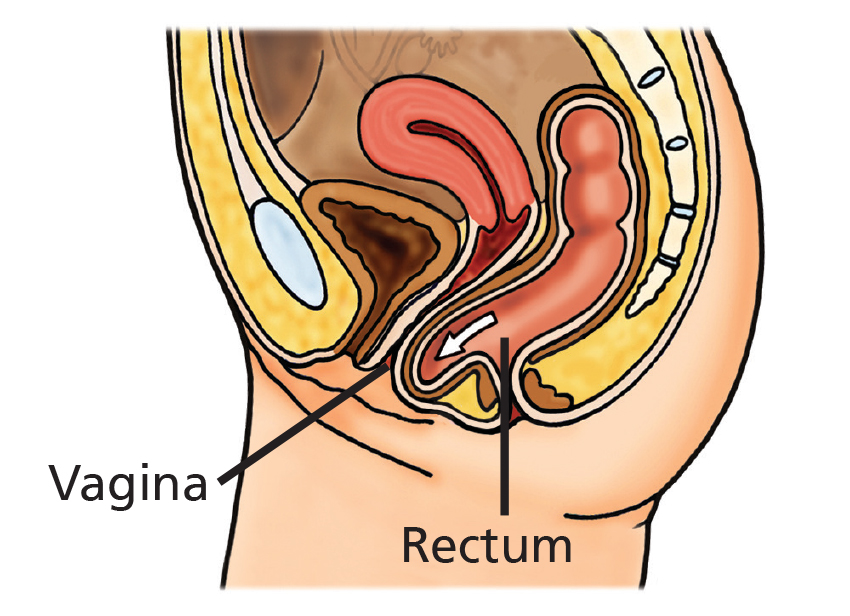
What is a pessary?
A pessary is a removable device which is inserted into the vagina to hold a prolapsed vaginal wall or uterus in place. Pessaries are made of Silicone and they come in different shapes and sizes.



How is the pessary fitted
A vaginal pessary is fitted by a nurse, physiotherapist or doctor. The initial fitting will be carried out in the clinic. A vaginal examination will be carried out to assess that the correct size and type of pessary is chosen. There are many different vaginal pessaries that can be used, the healthcare professional will choose the one best suited to you. After the vaginal pessary is fitted we will ask you to remain in the hospital to have a drink and pass urine. If that’s fine you’ll be able to go home.
A follow up appointment will be made for 4 months, so we can examine you and have a pessary replaced, if necessary.
Self-management of the pessary is an option, and if you chose this option you will be taught to remove, clean and reinsert the pessary yourself. Please ask your doctor if you are interested in this option.
What are the benefits?
- It may ease your symptoms and make you feel more comfortable, or they may go away completely.
- You may avoid surgery if the pessary resolves your symptoms.
- It can be used to make you more comfortable while you are waiting for surgery.
What are the risks?
You may experience some brief discomfort while the pessary is fitted. It is not uncommon to try a few different sizes and shapes before finding the one that is best for you. It is common to have a discharge with the pessary and that is normal. Please speak to your doctor if the discharge becomes very heavy or offensive.
Occasionally you might have a little spotting of blood following insertion of the pessary, however, this should settle quickly.
Long term risks include
- Ulceration of the vagina
This may give you abnormal bleeding or discharge. If you have bleeding you should see your doctor. Simply removing the pessary for a few weeks and using some Oestrogen cream in the vagina at night will often cure the problem.If it persists then you will be given a further hospital appointment for review. - Infection
If there is a smelly vaginal discharge a vaginal swab will be taken. The results will be reviewed. If treatment is required both you and your GP will be contacted so that treatment can be started. - Bleeding
If you report any bleeding you will be examined, and the ring may not be replaced. Following an assessment by a doctor you may need a pelvic ultrasound. Your pessary may be replaced on the advice of your doctor, depending on the results.
Can I have sexual intercourse?
It is possible to have sexual intercourse with the Ring pessary in place, although your partner may feel the pessary and you may have to experiment with different positions to find the most comfortable.
If you have a Shelf/Gellhorn pessary it is not possible to have sexual intercourse, this is because of the shape of the pessary.
What are the alternatives?
Do nothing
You can choose to do nothing if the prolapse is not causing any interference with daily life. However, avoiding heavy lifting or prolonged standing will reduce the symptoms.
Physiotherapy
Physiotherapy may help with the use of pelvic floor exercises, techniques and equipment aimed at stimulating and strengthening the pelvic floor muscles. The aim is to relieve any discomfort and in mild cases possibly “cure” the prolapse.
Surgery
The most common surgery for prolapse is a pelvic floor repair. This is a term used to describe basic repairs to the bulging vaginal walls. More specifically, the term anterior repair refers to correction of the front wall of the vagina; and posterior repair, to correction of the back wall of the vagina. If the uterus is prolapsing, then it can be removed with a vaginal hysterectomy. If you have already had a hysterectomy, then the top of the vagina can be re-suspended and supported.
What if the pessary falls out?
Sometimes the vaginal pessary falls out of the vagina. Do not worry – this simply means that the vaginal pessary is the wrong size and an alternative will be fitted at you next appointment.
Please contact your Consultant’s secretary so this can be arranged.