This leaflet is aimed at encouraging understanding of your condition and self-care. It can also be used to help others to provide care for you if needed.
Advice and videos to understand chronic swelling or lymphoedema and look after yourself. You should only complete this within your capability and comfort levels.
If you notice any signs of infection to your treatment area; such as redness, heat, swelling, discharge and you may feel unwell – seek medical attention by contacting your GP or 111 if out of hours.
What is Lymphoedema and chronic oedema
What is lymphoedema video by Pocket Medic Films- The circulation in your body is made up of a long series of connecting vessels and you probably have heard of veins and arteries supplying your body with oxygen and nutrients.
- Parts of this system will push fluid out deliberately, the fluid bathes your body tissues. The fluid is clear/ straw coloured.
- This fluid is usually collected and drained away by your ‘lymphatic system’ which is also a network of vessels but includes organs.
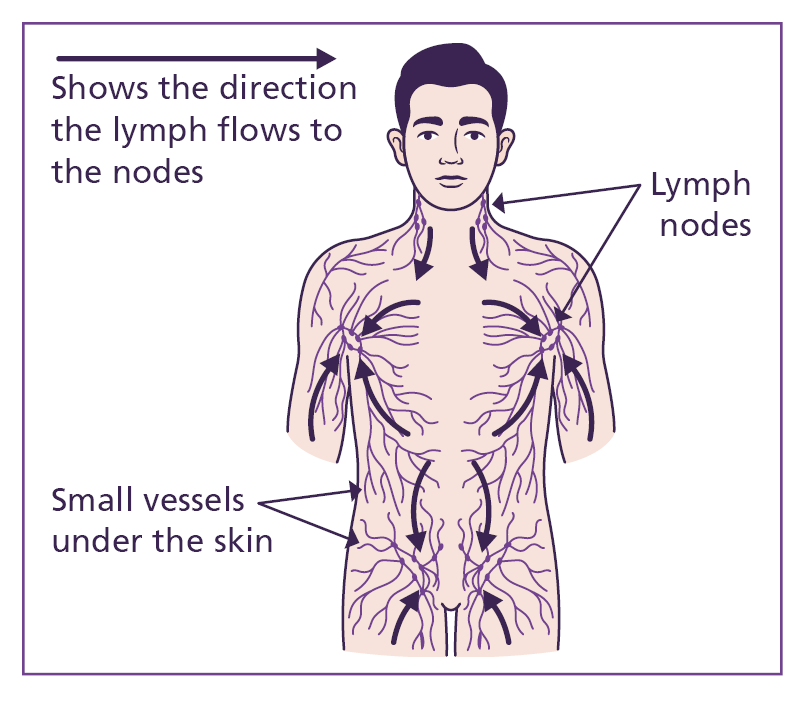
- The fluid will be filtered through lymph nodes (part of your immune system) to detect any invaders such as bacteria/ viruses. The nodes also filter out waste.
- During cancer treatment lymph nodes are often surgically removed and investigated to check whether cancer has spread to them.
- The clear fluid is called ‘lymph fluid’ and the lymphatics work together to move fluid back into your circulation where the fluid is passed out through kidneys or recycled within your body.
- Lymph vessels lie alongside but separate to veins and arteries.
- Whether you have been advised you have ‘chronic oedema’ or ‘lymphoedema’ you will have a swelling in part of your body that has been present for 3 months or more. Swelling is usually present in the limbs but can be present in any part of the body.
- Lymphoedema is when the lymphatics have failed/ or part missing/ or undeveloped resulting in a swelling.
- Chronic oedema is a symptom, and can be caused by many different health issues, which puts you ‘at risk’ of damage to the lymphatic system if left untreated. The lymphatics, in this case, are usually ‘failing’ because they’re struggling to keep up with the increase output from your circulatory system. Whichever you have the treatment is usually the same.
- With chronic oedema it is important to understand, and where possible, treat the underlying cause. For example: weight loss can improve lower limb circulation and drainage in turn reversing the symptom of chronic oedema.
- Lymphoedema can develop because the lymphatics did not develop properly during gestation (primary Lymphoedema) or damage to the lymphatics (secondary lymphoedema) such as cancer and/ or its treatment, suboptimal treatment of chronic oedema. If lymphatics are damaged they may be unable to collect fluid as they did before.
- There can be other causes for chronic oedema such as venous hypertension (varicose veins) and obesity, amongst others. In these instances, the lymphatics are usually overloaded and can be rectified by treating the underlying cause, for example, treating venous hypertension or losing weight.
- It is usually a mild swelling that can be managed, but some people develop a more serious swelling and need intensive treatment.
- Drugs and surgery are usually not the best way to treat the swelling.
- Self-care including physical treatments such as compression hosiery/ socks/ garments are proven and effective treatments to reduce swelling.
- Losing weight, if you are over-weight is very important, as compression will have limited effect if leg drainage is affected by a large abdomen.
- When lymphoedema develops after cancer treatment it often occurs within the first year but it may not develop until some years afterwards.
Cellulitis
Cellulitis video by Pocket Medic Films- This is an infection that affects the skin and tissues underneath.
- It is a problem with chronic oedema and lymphoedema because the immune system is not working as well as it should and struggles to fight the infection.
- Cellulitis often causes people to feel unwell, as though you are coming down with ‘flu’.
- If you notice any signs of infection to the affected area such as redness, heat, swelling and discharge and you may feel unwell you need to seek medical attention fast.
Skin care
Skin Care video by Pocket Medic Films- Wash the area carefully paying attention to folds and creases, pat dry rather than rub.
- Moisturise the swollen area every night with a proper moisturiser. Even if the skin looks in good condition, any slight area of dryness means that the top layer of skin is not completely intact. This means it can cause an entry point for bacteria, which can result in infection. Ensure the last application stroke is downwards to avoid clogging hair follicles.
- Avoid injury to your skin such as insect bites and trauma; this includes avoiding blood tests, injections, tattoos and piercings to the affected limb/ area.
- Check regularly for signs of redness, grazes and cuts. Clean any quickly with an antiseptic. If a sudden rash appears or an increase in swelling you may be experiencing cellulitis.
- Fungal infections will usually require treatment with an antifungal powder or cream.
Compression
Compression Garments video by Pocket Medic Films- Compression garments can help to prevent fluid from building up in the tissues and give support to muscles as they work.
- They provide pressure to help muscles pump fluid away from the swollen area during movement and exercise.
- Compression garments do not work well if ill fitting, old or worn.
- Your garments should ideally cover all swollen areas. You may require a combination such as a leg stocking and toe cap.
- You will probably find them easier to apply first thing in morning when there is less swelling.
- Aim to wear the entire day and avoid taking on and off as swelling can increase.
- Compression can generally be worn for up to 16 hours during the day and not advisable at night unless a Practitioner has advised.
- It is easier to apply garments over cool, dry skin.
- Application and removal aids are available to try if you are struggling to apply.
- Household rubber gloves may help you apply the garments easier.
- A slight sprinkling of talcum powder on the skin may help the garments to slide on.
- Do skin care regimes at night after garment removal. This helps prevent garment damage and ensures cream soaks in overnight.
Checklist for the day
- Is the garment spread evenly along your arm or leg so the pressure is even along your arm or leg.
- Remove creases and wrinkles. These act like elastic bands and cause fluid to build up behind them.
- Do not roll the top of the garment over.
- If the garment seems too long, use a rubber glove to ease the rest of the garment down the limb/ area.
- If the garment is tight and painful, remove and seek advice from your Practitioner, GP or District Nurse.
- If your toes turn a dusky blue colour remove and seek advice from your Practitioner, GP or District Nurse.
- If the garment is loose it probably isn’t fitting or working well. You probably need a different size.
- When you receive new garments, throw away old ones to ensure you always wear the best supporting ones.
Do not wear compression if;
– You notice your limb turning a dusky blue/ mottled colour.
– Experiencing pins and needles.
– Experiencing numbness.
– Limb has become cold associated with poor circulation.
– Seek medical advice in these instances.
Activity and movement
Cancer Research UK webpage ‘Exercise, positioning, and lymphoedema’- A separate patient information leaflet is available to advise on activity and movement for your particular area of swelling.
- Our focus is always to optimise self-care and enablement.
Weight loss
NHS Patient Webinars on Weight Management- Swelling is more difficult to control if you are overweight.
- A large abdomen can cause lower limb circulation to become dysfunctional.
- Sitting for prolonged periods kinks the groin which can cause lower limb circulation to become dysfunctional.
- Recliner chairs can still cause the groin to kink.
- Lying flat with your legs raised, as long as there is no restriction to breathing, is a good way to help leg drainage.
- A large central body mass and large arms also can restrict upper limb circulation and drainage.
Eating habits
- Try to reduce your intake of high fat and processed foods.
- Eat plenty of fresh fruit and vegetables.
- Water and fruit juices are better alternatives to tea, coffee and sugary drinks.
- A ‘Helping with Weight Loss’ patient information leaflet is also available with some useful ideas.
- Restricting water intake is not recommended. This will not help to reduce lymphoedema or chronic oedema and could be harmful.
Website links
NHS Patient Webinars on Weight Management Pocket Medic webpage on LymphoedemaPocket Medic – all videos used with permission from Pocket Medic. Information taken 06/12/2024. Videos produced by Lymphoedema network Wales.
Cancer Research UK webpage ‘Exercise, positioning, and lymphoedema’All videos and narrative used with permission from Cancer research UK website. Cancer research are independent from Leeds Teaching Hospitals. ©Cancer Research UK [2002] All right reserved. Information taken 06/12/2024
Useful addresses and phone numbers
Contact Numbers for Leeds Cancer Support
Information lounge level Minus 2 Radiotherapy department
Open Monday to Friday from 8:00am – 6:00pm
Tel: (0113) 206 7603
Information centre Level 1 Outpatients department
Open Monday to Friday from 10:00am – 4:00pm
Tel: (0113) 206 8816
Sir Robert Ogden Macmillan centre
Open Monday to Friday from 10:00am – 4:00pm
Tel: (0113) 206 6498
All above services can be emailed on: [email protected]
You can contact the Lymphoedema department Monday to Friday during the day. Hours can vary; Tel: 0113 392 1807