This leaflet has been produced to advise you and your relatives how to keep your skin healthy whilst in hospital, some information will also be helpful when you are discharged home.

– Surface
– Skin Inspection
– Keep Moving
– Incontinence
– Nutrition & Hydration
What is a pressure ulcer?
Pressure ulcers, also known as bed sores, are areas of damage to the skin and tissues below caused by sitting or lying in one position for too long. They can also be caused by ill-fitting footwear; sliding down the bed; inappropriate wheel/armchairs and poor personal hygiene.
Who is at risk?
Some people are always at risk of developing a pressure ulcer. Everyone is at some risk in hospital because they move around less. This could be due to tiredness, medications or pain.
You are more at risk if you:
- Have poor or restricted mobility for example staying in one position in bed or in a chair for a long period of time without moving.
- Currently have a pressure ulcer or previously had a pressure ulcer.
- Have a loss or lack of feeling or sensation in your skin which may be due to diseases such as multiple sclerosis, diabetes, stroke, poor circulation, heart disease, vascular or blood vessel diseases.
- Are on strong pain killers such as morphine or have an epidural in place.
- Have memory problems.
- Don’t eat or drink enough.
- Are overweight or underweight.
- Have vulnerable skin, e.g., dry, moist, paper thin, redness.
- Have a low mood or emotional status which can lead to inactivity.
Skin inspection – get to know your pressure areas
If you have been assessed by the nurses as being at risk for one or more of the above reasons they will ask to check your skin over these vulnerable areas once per shift.
Lying on your back
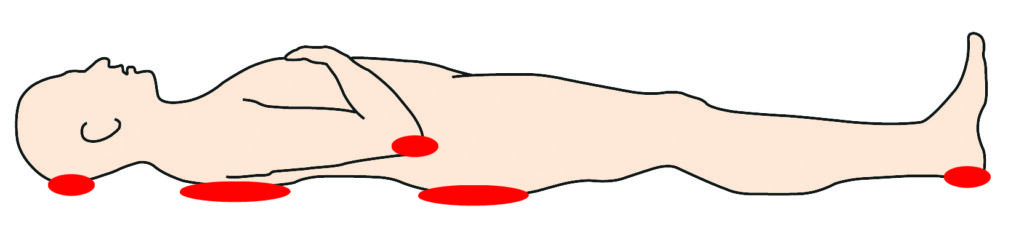
Lying on your side
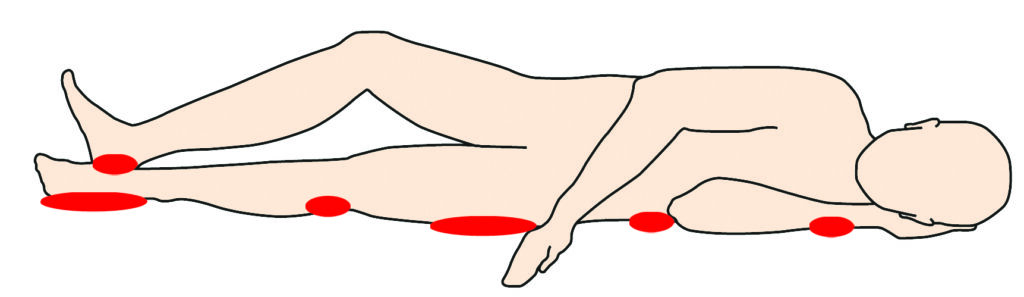
Sitting up in bed
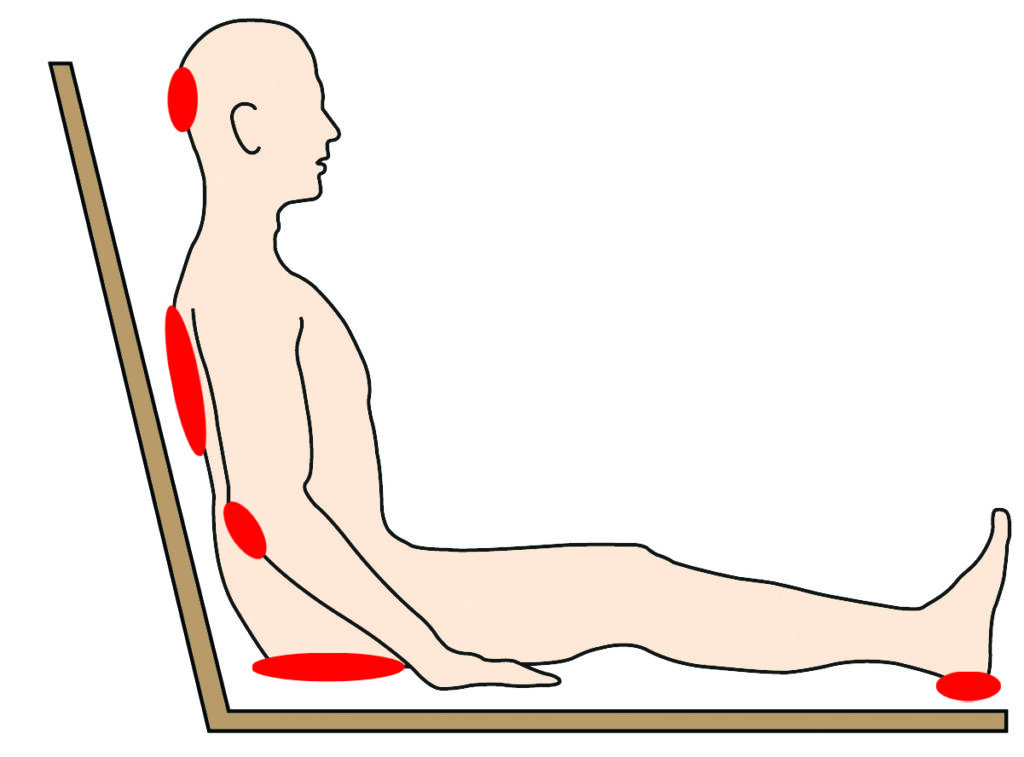
Sitting in a chair or wheelchair
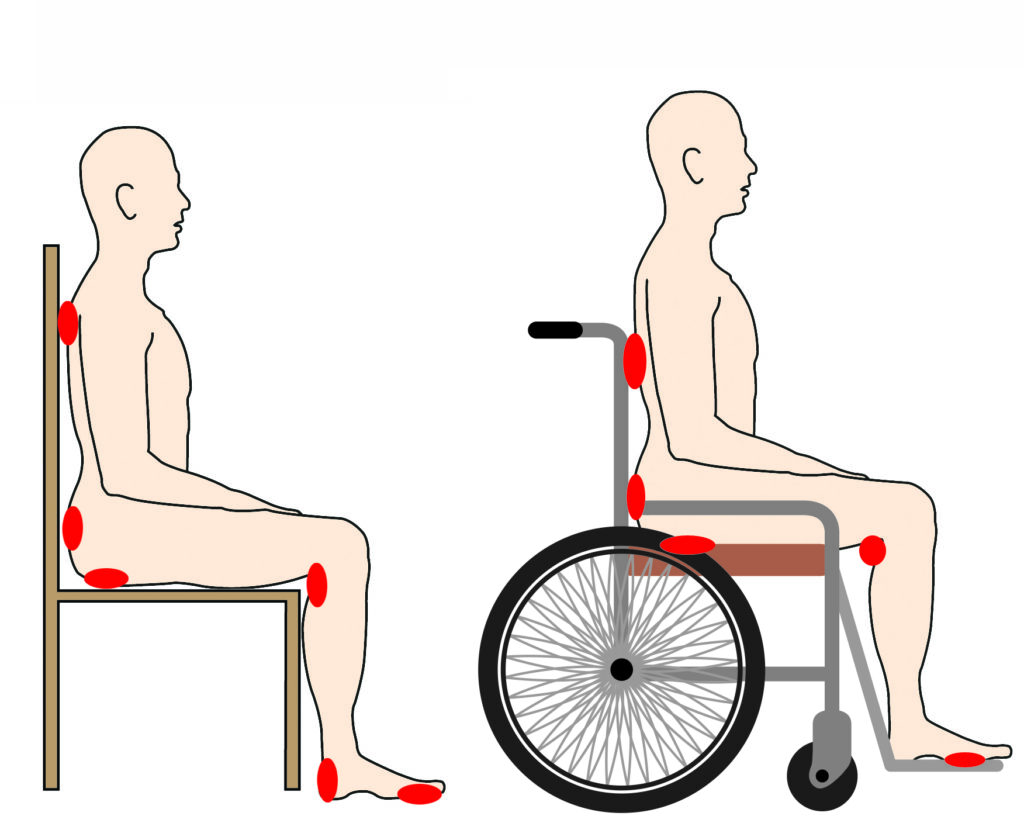
Surface
Pressure relieving equipment may help reduce this risk.
These may include a mattress or a chair cushion, to help reduce the amount of pressure on your body. Please inform the nursing staff if the equipment you have been provided with is not working or is uncomfortable. Also let staff know if you normally use a special cushion or mattress at home.
Patient quote
“I am pleased I told the nurses that my father had a special mattress at home because they got him one straight away.”
Pressure ulcers can also occur under medical devices used to treat your condition. For example, an oxygen mask, tubing, catheter, cast or neck collar. It is important that you inform the nursing staff if you have a poorly fitting or painful medical device.
Keep Moving
If you have been identified as being at risk of developing a pressure ulcer this may be because of reduced mobility.
Regular movement is key to prevention, whether you’re in bed or sat out in a chair. Ask the nurses to help you move.
By moving side to side and lifting the bottom, pressure is relieved for a short time.
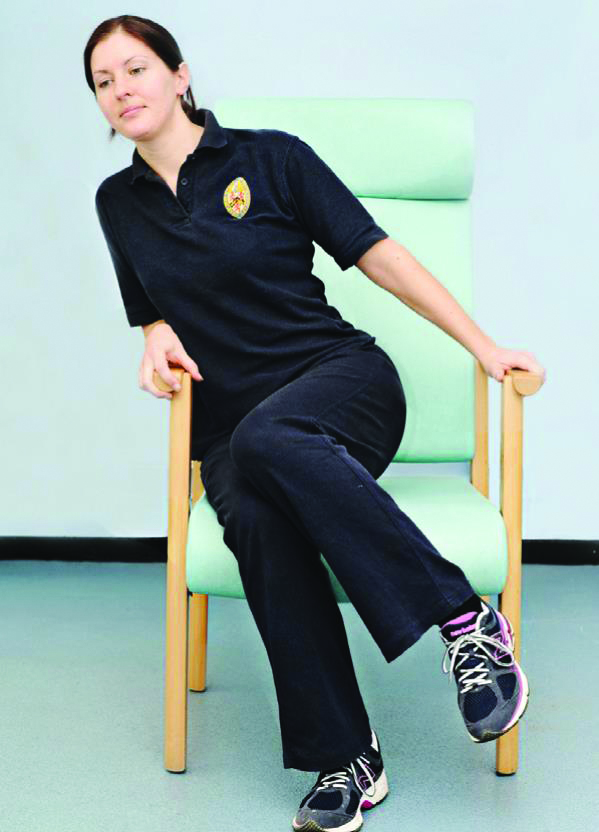
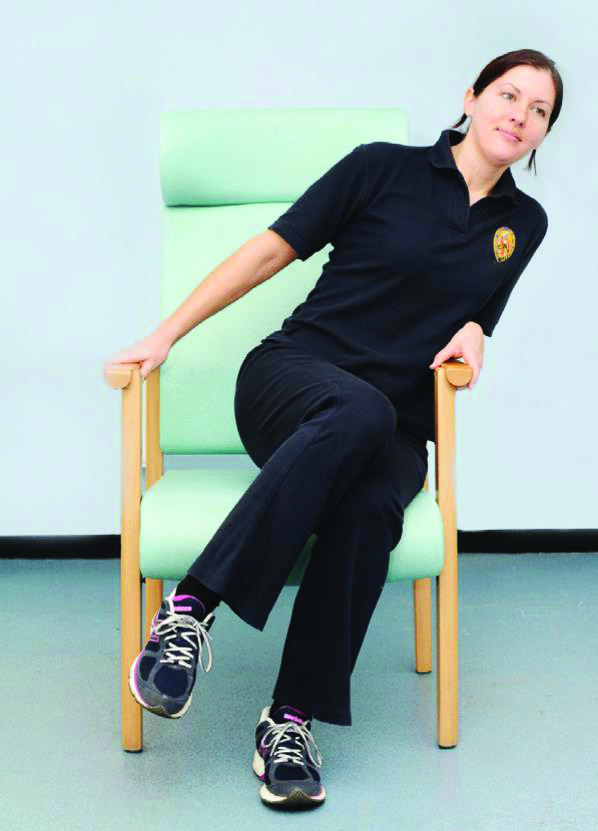
Good posture helps to spread the weight of the person and reduces pressure on bony areas. Lift the bottom regularly if you are safe to do so to relieve pressure. Use your call bell if you need assistance with this.
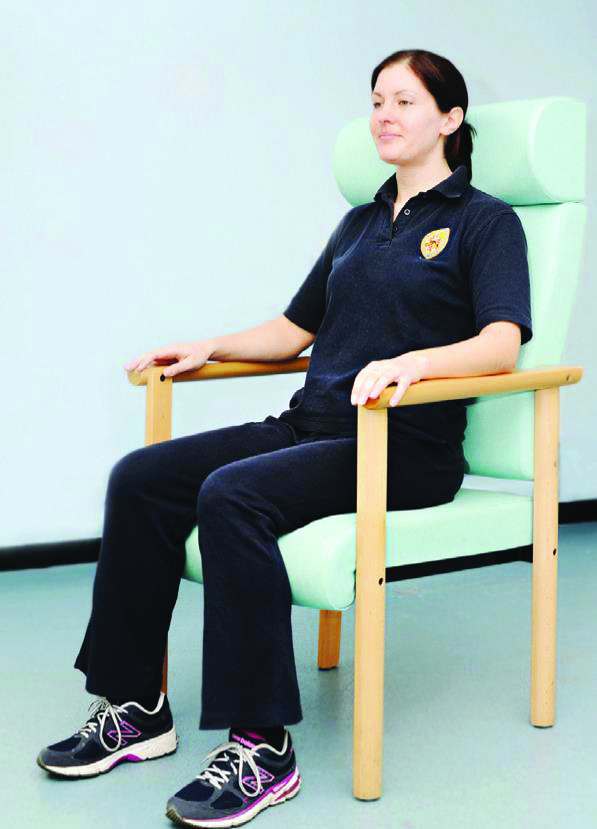
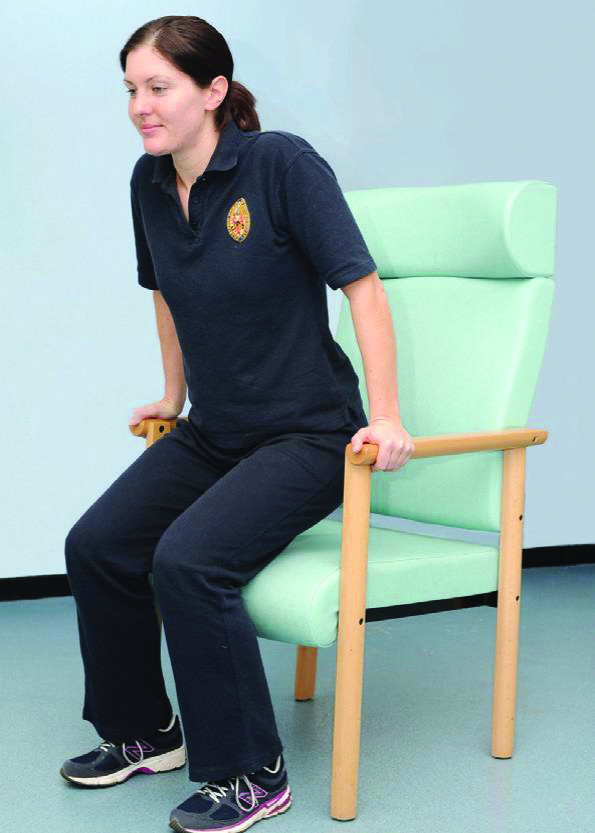
Reference: Pressure Ulcer Prevention
Images used with kind permission of Catherine Cross – Physiotherapist.
Incontinence
Too much moisture can be damaging to the skin, for example urine, faeces or sweat. Moisture, shear (sliding) and friction can all increase the risk of developing a pressure ulcer and make skin more vulnerable.
Please tell the nursing staff if you are having incontinence problems as there may be aids, we can provide which can help to manage this, for example pads. The nursing staff can also refer you to the Continence Promotion Team for advice.
Keep skin clean, dry and moisturised. Good personal hygiene is important. A foam cleanser can help to keep skin clean, and a barrier product protects the skin. Ensure your skin is patted dry not rubbed after cleaning.
Staff quote
“I would be so upset if one my patient’s developed a pressure ulcer, I make sure everyone looking after them knows if someone is at risk, all staff have a role to play.”
Nutrition and Hydration
Your risk of developing a pressure ulcer is increased if you are not eating and drinking as much as you would do normally.
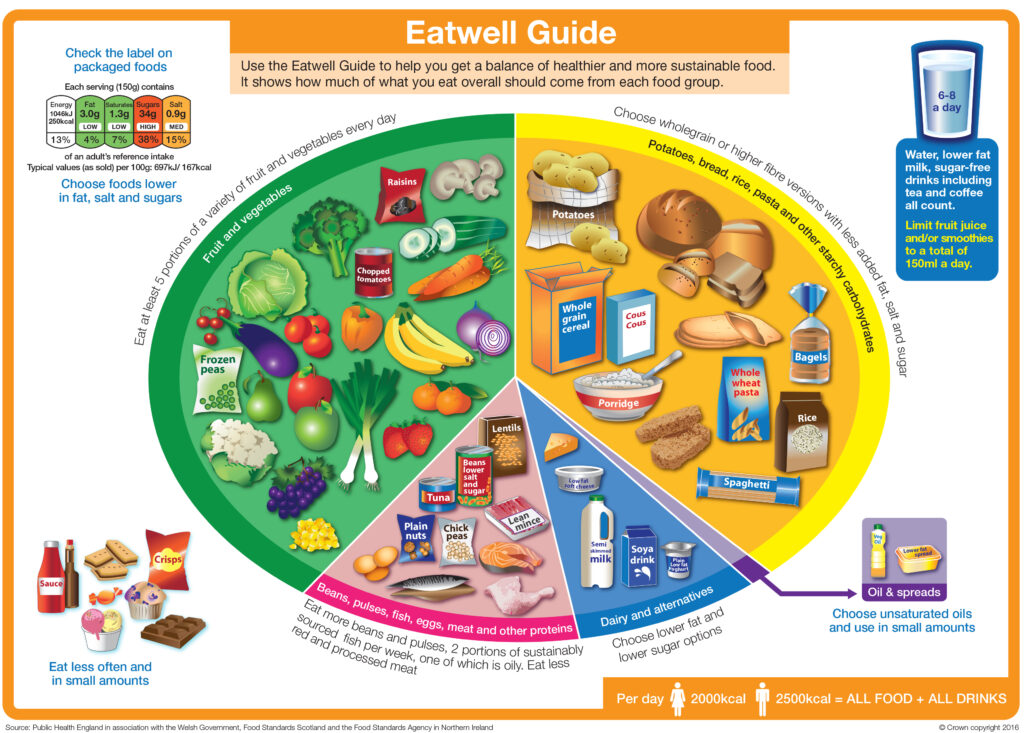
You should be drinking at least 6 to 8 drinks a day to help keep your skin healthy. This can include a mix of the following: water, juice, squash, tea, coffee, decaffeinated or milky drinks.
Weight loss can increase your risk of skin breakdown. Being underweight or overweight can also increase your risk.
Staff will monitor your weight when you first come into hospital and weekly. If staff have any concerns or if you already have a pressure ulcer, you may be given supplement drinks or referred to the Dietitian.
There are lots of different menus available to meet cultural, religious or medical needs. See the leaflet eating well for wound healing and preventing skin breakdown.
Smoking damages blood vessels and affects overall skin health and circulation. If your skin is at risk, it is advisable to stop smoking.
Remember, it’s important to look after your skin by:
- Moving regularly.
- Eating and drinking well.
- Telling staff if you have any pain or discomfort.
There is a leaflet available: Staying Active In Hospital.
If you would like any more information or have any concerns, please speak to a staff member on the ward.
Staff can refer you to the Tissue Viability Service, Physiotherapists, Dietitians and Occupational Therapists if your needs are complex or if your condition is deteriorating.
Patient quote
“I am glad I told the nurses that my bottom was sore, because we caught the ulcer early.