Following major gynaecological surgery, many patients have traditionally remained in hospital for 5-7 days. It has been shown that by altering how patients are managed both before and after surgery, they can be safely discharged home in 4-5 days.
Patients having laparoscopic (keyhole) or robotic surgery may be discharged home the following day. In order to achieve this, we ask you to play an active part in your recovery. This booklet explains what will happen to you and what you can do to help.
Important
It is important that you access this information when you come in for your operation. It will guide you through what will happen each day on the ward.
Before your operation
Smoking
We strongly advise that you stop smoking before your surgery. The longer you are smoke free before your operation, the better. Continuing to smoke before surgery can increase the risk of complications involving your heart, lungs and surgical wounds. Any of these may result in you having a slower recovery and a longer stay in hospital.
- Your GP will be able to give you advice and prescribe Nicotine Replacement Therapy (NRT) if appropriate.
- You can buy NRT over the counter at your local pharmacy.
- You can contact your local stop smoking service which provides free, friendly support.
Exercise
You should try to remain active. Regular gentle exercise, such as walking, will be of benefit to your heart and lungs as well as helping your body to cope with the effects of an operation.
Nutrition
It is important to eat a healthy diet in the time leading up to your operation. This will help with your recovery after surgery to heal wounds and reduce your risk of infections. If you are finding it difficult to eat you may benefit from taking some nutritional supplement drinks. You can get these from your local pharmacy or on prescription from your GP. Eating little and often may also help.
Diabetes
If you are diabetic it is important that your diabetes is well controlled. You should try to stick to your diabetic diet and make sure that your blood sugar levels are stable. It may be necessary to see your GP for review if your diabetes is not well controlled. High blood sugars can delay wound healing and increase your risk of infections.
Bowels
You should try to avoid being constipated when you come in for your operation. Eat foods high in fibre (eg fruit, vegetables, brown bread/rice and wholemeal pasta). Drink plenty of fluids and take regular exercise. See your GP if you feel you need medication (laxatives) to help.
Pre-assessment clinic
You will be sent a medical history questionnaire by text to your mobile phone, which you will be asked to complete and send back by text. You will be asked about your general health, previous operations/illnesses, allergies and any medication that you take. If the pre assessment team don’t receive the questionnaire back (if maybe your mobile doesn’t accept such texts) or if you don’t have a mobile then the pre assessment nurses will ring you and go through the questions over the phone.
You will be asked to attend the pre assessment clinic so they can record your height, weight and blood pressure and take some blood tests. You may also need an ECG (heart tracing) if needed. Some patients are given bowel preparation and/or carbohydrate drinks (see later in this leaflet).
Staphylococcus Aureus is a type of bacteria that commonly lives in the nose and on the skin. You will be assessed to see if you are at risk of having this bacteria and may be given some treatment by the pre assessment team. This consists of a body and hair wash to use before surgery and also some cream to put at the base of your nostrils. You will be given instructions on how to use it if needed (not everyone will need this treatment).
The clinic is an opportunity for you to tell us about your individual needs and circumstances. If you are worried about managing at home after your operation it is important for you to tell us as early as possible. We have a team of healthcare professionals who can help organise any relevant support you might need. These include physiotherapists, occupational therapists, social workers and discharge co-ordinators.
Carbohydrate drinks and Bowel Preparation
You may be given some carbohydrate drinks, called Preload, to take before your operation. These drinks will increase the amount of carbohydrate stored in your body which can help your recovery after surgery. Not all patients will need them as it depends on the surgery you are having. You will be given either two or three sachets of Preload depending on your medical history (we don’t give them at all to diabetic patients) and they are provided by the pre assessment team with written instructions.
Each sachet should be dissolved in 400 mls of water. You take the first two sachets the evening before surgery from about 5pm. If you have a third sachet then you should take it at 6am on the morning of surgery (this replaces the glass of water that your admission letter may say to take at 6am).
A small number of patients may be given some ‘bowel prep’ drinks to have the afternoon and evening before surgery to empty their bowels at home. This is usually two sachets of Citrafleet.
Each sachet of powder is dissolved in a glass of water. They will be given out by the pre assessment team if your consultant surgeon has requested it and you will be given written instructions on how to take them. Sometimes patients are admitted to the ward the day before surgery to have this bowel prep.
Admission and Fasting
Most of our patients are admitted to hospital on the day of their surgery at either 7am (for a morning or all day theatre list) or 11am (for an afternoon list).
You will be asked to go to either the David Beevers Unit (ground floor of Lincoln Wing) or the Admission Lounge (2nd floor of Lincoln Wing) to be admitted and prepared for surgery. Your admission letter will tell you when to fast from. Fasting means you will not be able to have anything to eat or drink after a specific time.
Fasting times vary and will depend on whether your surgery is in the morning or afternoon.
Important
You must stop eating food six hours before your operation; this includes mints, chewing gum, boiled sweets and tea/ coffee with milk or sugar. Water must be stopped two hours before your operation. You will be told to have 250mls of water just before you stop drinking. If you are unsure about your fasting instructions then please contact your surgeon’s secretary.
Medications
Before you are admitted to hospital, please make sure you have ordered enough supplies of your regular medicines to last during your recovery period. We suggest you have at least two weeks supply of these medicines at home. We do not supply your regular medicines to take home.
Please bring a supply of each of your medicines with you. This should include those you take regularly and any you only use when you need them. This may include tablets, inhalers, sprays, patches or injections that you get from your GP, a hospital or ones you buy yourself. If you have a repeat prescription list from your GP please bring it with you.
In most cases, you will continue taking your usual medicines during your hospital stay, using your own supplies. Any changes to your medicines will be explained to you before you leave hospital. You will take any remaining medicines home with you.
If we start you on any new medicines, we will give you a supply of these to take home, along with the information about how to take them.
Whilst you are in hospital you will be given an injection of heparin every day. This helps to reduce your risk of blood clots (thrombosis). The injections are usually needed for 28 days (occasionally only 7 depending on your surgery) and you will need to continue them at home. You can be taught how to give these injections yourself or someone else such as a family member can do it for you.
Important
If you are taking Aspirin, Warfarin, Dipyridamole, Clopidogrel, Apixaban, Rivaroxiban or Dabigatran medication you must tell the pre-assessment team and your doctor as they will usually need to be stopped before your operation.
Please ask a member of staff if you have any questions about any of your medicines.
Pain control
Effective pain control is an essential part of the enhanced recovery programme. This will help you to start walking around, breathe deeply, eat and drink, feel relaxed and sleep well.
You may be offered a patient controlled analgesia (PCA) pump which allows you to control your pain relief yourself. A hand held button is connected to the pump which contains a strong pain relieving medication (usually oxycodone). When you press the button, you are given a small amount of the medication through a drip in your arm or hand. There is a security device that stops you from having too much.
Along with your PCA, you may also be given some local anaesthetic to numb the area over your wound.
This can be injected near to your wound while you are still asleep in theatre and would last for a number of hours. Alternatively, you may be offered a system where local anaesthetic is infused continuously around your wound for up to 72 hours. With this system you have two thin tubes inserted down each side of your wound while you are asleep in theatre. These tubes are attached to a pump which contains the anaesthetic.
Alternatively, you may be suitable for an epidural to provide pain relief after your operation. This is a small tube in your back which provides a small, measured, continuous supply of pain relieving medication. This should numb the area over your wound and can continue for up to two days depending on your recovery.
Your anaesthetist and surgeon will discuss pain relief with you before your operation.
The nursing staff will check that you are comfortable. They will ask you if you have pain and will ask what your pain score is. This is on a scale of 0-3 where 0 is no pain and 3 is severe pain. This allows the staff to check that your pain medication is working for you.
Once you are feeling better your PCA and/or local anaesthetic pump or epidural will be removed and you will be given other pain medication to take by mouth. If you have any nausea (feeling sick), then please speak to your nurse who will be able to give you medication to help.
Breathing and circulation exercises
Following your operation, when you wake up, it is important that you do deep breathing exercises. With your shoulders relaxed, take a deep breath in, hold for 1-2 seconds and then let the breath out. This should be done at least five times an hour.
You should also do exercises to help your circulation and reduce the risk of blood clots. Circle your ankles both ways and then point your toes up towards you and then back down briskly. Ten of these exercises each hour would be beneficial until you are walking regularly. Moving around has been shown to reduce your hospital stay. It helps the bowel to get working and encourages a feeling of well-being for you.
You will be asked to wear compression stockings, which can also help to reduce your risk of blood clots. You will be asked to wear them day and night for two weeks but can remove them for showers. We will give you a spare pair when you go home.
Coughing
After your surgery, it is important to keep your chest clear by coughing up any phlegm or mucus that is produced by the lungs. This is especially important if you are, or have been a smoker. This will help minimise the chances of you developing a chest infection. Being in pain will prevent you from coughing effectively, so it is vital that your pain is controlled enough to allow you to cough. If the pain is too severe, you must inform the nursing staff who will alter your pain relief medication.
Your wound is designed to withstand the pressure of coughing, so don’t worry about doing any damage. It is easier to cough if you sit forward and if you use your hands pressed firmly over the wound to support your coughing muscles.
Please practice these exercises at home before your operation so you become familiar with them.
Day of surgery – what to expect
The following information is a guide only. Everyone recovers from surgery at a different rate so do not worry if you feel you are not achieving the goals described.
Before surgery
- You will be given a theatre gown, paper knickers and compression stockings (to reduce your risk of blood clots).
- Wigs or headscarves can be left on. Headscarves may be more comfortable as you may get very hot wearing a wig.
- You must remove make-up, nail polish and jewellery (sentimental rings can be covered with tape). Piercings usually need to be removed – please check before you are admitted to hospital.
- You will need to remove contact lenses. Glasses, dentures and hearing aids can be left in place until you enter theatres and then put back on or in as soon as you are awake after your surgery.
- You will see your surgeon and anaesthetist on the ward before your surgery.
After surgery
- You may have a drip in your arm to give you some fluid to make sure you do not become dehydrated.
- You may also have a catheter (tube) in your bladder to help you pass urine.
- You may have an epidural, local anaesthetic infusion or PCA from theatre and regular pain relief tablets will be prescribed.
- A few hours after your surgery, depending on the extent of your operation, you may be able to sit out in a chair for a short time and walk if comfortable. This is usually if you have had laparoscopic (keyhole) or robotic surgery. If you return to the ward later in the evening it may be the following morning before you sit out in a chair. The nurses will help you do this. Please do not attempt this on your own.
- A few hours after your operation you may be able to start drinking. You may even have something light to eat if you are not feeling nauseous. Your doctor or nurse will advise you on this.
- You may be able to go home today if you have had laparoscopic (keyhole) or robotic surgery.
It is important to do your ankle and deep breathing exercises. This will help to reduce the risk of blood clots such as Deep Vein Thrombosis (DVT) and prevent chest complications.
Day 1 after surgery – what to expect
- You should eat and drink as advised, as much as you feel able to. Please ask for anti-sickness medications if you feel sickly.
- If you have a drip and/or catheter, they may be removed today.
- If you have a PCA or epidural, this may be removed later today if you can manage to use pain relief tablets.
- You will be assisted to have a wash and if you feel well enough, get dressed.
- Today you can sit out in a chair for at least six hours, with rests on the bed in between as you need.
- If you were able to walk easily before your operation, you will be encouraged to walk along the ward corridor and back at least four times as this helps with digestion and reduces the risk of blood clots, chest infections and constipation. Please do not attempt this on your own if you have an epidural or PCA pump as the nurses will assist you. It is important to do your ankle and deep breathing exercises. This will help to reduce the risk of blood clots such as DVT and prevent chest complications.
- You may be able to go home if you have had laparoscopic (keyhole) or robotic surgery.
Day 2 after surgery – what to expect
- Continue to eat and drink as you can tolerate. You should try to drink 1-2 litres in the day.
- For pain relief you may still have a PCA pump, a local anaesthetic infusion device or an epidural from theatre. This may be removed today and regular pain relief tablets will be prescribed.
Tell the nurses at any point if you are in pain. It is important to take regular pain medication so you can walk around the ward, help care for yourself and eat your meals comfortably. - Your catheter may be removed today if you are able to mobilise to the toilet. Patients who have had a trachelectomy or radical hysterectomy usually keep their catheter in for a few more days.
- Trapped wind and wind pain is very common after surgery. Walk around as much as possible to help relieve this. Peppermint tea / capsules can help too. Wind usually begins to improve once bowels have opened.
- You should be feeling much more independent today, able to take a shower and get dressed. Please ask a nurse for assistance if required.
- You can sit out in a chair for a total of eight hours, with short periods of rest on the bed.
- If you were able to walk easily before your operation, you will be encouraged to walk along the ward corridor and back at least four times.
- Your doctor should be able to give you an idea of when you can go home.
Please note
It is important to do ankle and deep breathing exercises. This will help to reduce the risk of blood clots such as DVT and prevent chest complications.
Day 3-5 after Surgery – what to expect
- Continue to eat and drink as you can tolerate. You should try to drink 1-2 litres in the day.
- You will be encouraged to be independent with your hygiene needs such as showering and getting dressed.
- You can sit out in a chair each day for a total of eight hours, with short periods of rest on the bed.
- If you were able to walk easily before your operation, you will be encouraged to walk along the ward corridor and back at least 6 times.
Helpful Hint
Walking after meals helps with digestion and may relieve wind pain.
You will be seen by your gynaecological team on a daily basis and they will allow you to go home if:
- You feel confident about going home.
- You are eating and drinking enough.
- You are walking round the ward fairly comfortably.
- You do not have a temperature or any signs of an infection.
- You are passing urine without difficulty.
- You are passing wind. For some patients the doctors will also require you to have opened your bowels before going home.
Please note
It is important to do ankle and deep breathing exercises. This will help to reduce the risk of blood clots such as DVT and prevent chest complications.
Getting ready for going home
Once you are well enough to go home we will aim to have everything ready for you to leave the ward by 12 midday. If you are being picked up by a relative or friend please let them know as soon as possible so that they can be available for you. You will be given a number of medications to go home with, including pain relief tablets and heparin injections to help to prevent blood clots such as DVT.
You can be taught how to give these injections yourself or someone else such as a family member can do it for you. We will give you a sharps bin to put the used injection syringes in. When you have completed your course please take the sharps bin to your local chemist/ pharmacy and they will dispose of it.
What happens when you go home?
Continue to take your pain relief medication regularly at home as long as you need to. This will allow you to move around easily, breathe deeply, eat, drink and sleep well. Try to have a shower or bath every day. You may find it easier to shower at first as it can be painful getting in and out of a bath. If you do have a bath, consider kneeling in it, as you may find it easier to get out.
If you are prescribed heparin injections then ensure you have them every day as prescribed until you have finished the course. This is extremely important to reduce your risk of developing blood clots. Continue to move around regularly to reduce your risk of blood clots, chest infections and constipation. Walk around your house several times a day.
Have a 10-15 minute walk outside every day and then slowly increase this time over the next few weeks until you are back to your normal level of activity. If you were not able to walk far before your surgery then do as much as you feel able to.
If you have a ‘Honeycomb’ wound dressing you will be asked to remove it on the fifth day after surgery. It is easier to do so after a shower. If you have a specialist PICO dressing this can also be removed after a shower but on the eighth day after surgery. If you have had laparoscopic or robotic surgery then the small dressings can be removed on the third day after surgery. The ward staff will tell you which dressing you have. Your stitches are usually dissolvable so do not need to be removed. If you do have non-dissolvable stitches or staples, the ward will arrange a community nurse to remove them.
Complications and side-effects following your surgery
Complications happen occasionally so it is important that you know what to look out for. Please contact your GP or specialist nurse for advice if you feel you have any problems. You can also call ward J98 for advice.
Vaginal bleeding
It is not unusual to have some vaginal bleeding or a blood stained discharge after your operation. This can last up to six weeks. If you are worried that the bleeding is continuing, becoming heavier or is offensive (smelly) please contact your GP or specialist nurse for advice.
Your wound
It is not unusual for your wound to be slightly red and uncomfortable during the first one or two weeks. Please contact your GP if your wound:
- Becomes inflamed, painful or swollen.
- Starts to discharge fluid.
Your bowels
Your bowel habit may change following your operation and may become loose or constipated. Make sure you eat regular meals three times a day, drink plenty of fluids, and take regular walks. This is especially important for the first few weeks after your operation.
Eat foods high in fibre such as fruit, vegetables, wholewheat cereals and brown bread/ rice/pasta. You may be prescribed a gentle laxative to take at home but you can speak to your GP if you feel you need a different one. Please note that it can take 2-4 weeks for your bowel to act normally.
Passing urine
Once you have your catheter removed. Your bladder function can sometimes change for a few weeks after surgery. You may find that it takes longer to pass urine or feel that your bladder is not emptying fully. Rocking gently backwards and forwards or side to side whilst sat on the toilet can help to fully empty your bladder.
Occasionally you may not be able to tell when your bladder is full so you will need to make sure that you go to the toilet regularly to try and pass urine. All of these things usually improve over time. Keep an eye on the colour of your urine. If you have had plenty of fluids it should be pale yellow.
If your urine is darker, it may be a sign that you are dehydrated and you should drink more.
Important
If you have a stinging/burning sensation when passing urine or you are passing small amounts of urine very frequently, please see your GP as you may have an infection.
Blood clots
If you experience tenderness, swelling, redness, warmth or pain in your lower leg then you could have a deep vein thrombosis so you should ring your GP or visit the Accident and Emergency (A&E) department as soon as possible.
Important
If you suddenly develop shortness of breath, chest pain or are coughing up blood then ring 999 as you could have a pulmonary embolism which is a medical emergency.
Looking after yourself
Diet
A balanced, varied diet is recommended to help your body recover. Try eating small amounts three or more times a day. If you are finding it difficult to eat, you can supplement your food with three to four nourishing, high protein, high calorie drinks such as Fortisip or Complan.
These are available from supermarkets and chemists. If you are losing weight without trying to or are struggling to eat enough, your GP or consultant may refer you to a dietitian for further help and advice.
Household Activities, Hobbies and Exercise
You should avoid vacuum cleaning, ironing, laundry and carrying heavy shopping bags for 4-6 weeks after your operation. However you can use a kettle (don’t overfill it), make yourself meals (try preparing food sat down) use small pans on your hob and do a small amount of washing-up if you wish. You can also use the stairs freely as this won’t affect your wound. You should consider taking up your hobbies and activities as soon as possible after surgery if they are not too strenuous.
Getting back to regular activities can help your emotional recovery as it is a form of normality for you. We recommend you walk outside regularly and gradually build this up over the next few weeks.
Swimming can be resumed in 4-6 weeks if vaginal bleeding has settled. Yoga, pilates and exercises involving weights need to be avoided for at least 12 weeks and then restarted gently.
For more advice about specific activities please speak to your surgeon or the ward physiotherapist.
Common sense will guide your exercise and rehabilitation. In general, if your wound is still uncomfortable, modify your exercise. Once the wounds are pain free you can return to your normal activities.
Work
You may be able to return to work 4-12 weeks after your operation depending upon your surgery, recovery and type of job. Your surgeon, ward nurse or physiotherapist will be able to advise you further. If you require further treatment after surgery then you will likely need longer off work.
Driving
You should not drive until you are confident that you can drive safely. A good measure for this is when you have got back to most of your normal activities. Your surgeon may give you specific advice in hospital as to when you can drive again but otherwise this will usually be within 6 weeks after surgery.
It is important that any pain has resolved to enable you to perform an emergency stop and turn the wheel quickly. It is also advisable to check your policy details with your insurance provider.
Sex and relationships
Undergoing surgery can be upsetting and emotionally draining. The support from partners and close friends can be of great help in order to cope with everything you are
faced with. Having surgery may affect your sexual life and may also cause a loss of sexual desire.
This can be temporary and usually improves in time together with the support and understanding of your partner. You may resume sexual activity around 6 weeks after surgery if you are comfortable and have returned to your usual activities.
If you need further support or advice at any point please contact your clinical nurse specialist team who will be happy to discuss your concerns with you.
Physiotherapy Exercises
Pelvic Floor and Deep Abdominal Muscles work together to support the pelvic organs and pelvis itself. Strong muscles can maintain or improve bladder and bowel control, help to prevent prolapses and help to protect the back.
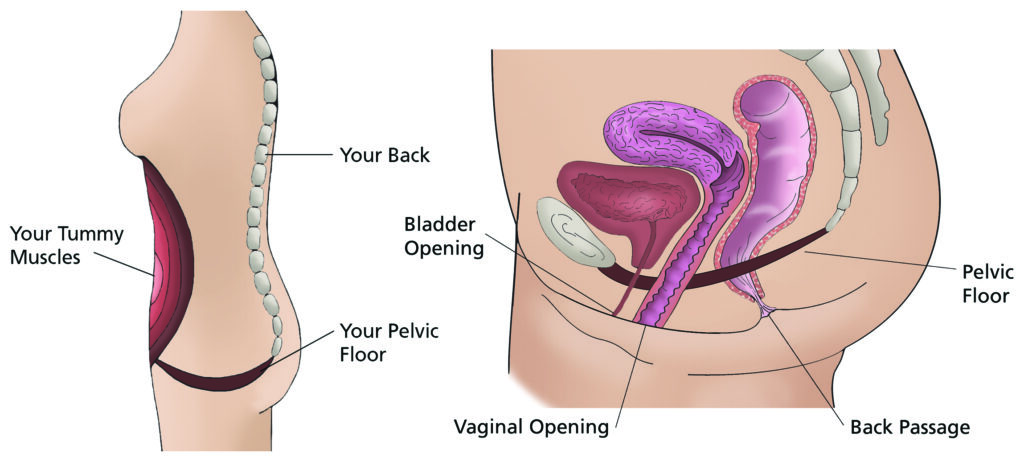
Pelvic Floor Exercises
Do in any position and start as soon as you feel comfortable. If you have a catheter, wait until it has been removed.
- Imagine trying to stop yourself from passing wind and at the same time trying to stop the flow of urine.
- You should feel a squeeze and lift – a drawing up feeling inside.
- Hold this squeeze and lift for a few seconds and then relax, repeat a few times.
- Don’t worry if you can’t feel it at first. As you improve, hold as long as you can (up to 10 seconds) and increase the repetitions (up to 10 times).
- Do not exercise by stopping your urine flow midstream – it could damage your bladder and lead to infections.
Quick Pelvic Floor Contractions
Squeeze strongly and relax immediately, allow a few seconds to relax, then repeat as many times as you can up to 10.
Deep Abdominal Muscle Exercises
This muscle is like your natural corset and will help to support your back.
You can do this exercise in any position, but keep your back straight.
- Let your tummy sag and breathe in gently.
- As you breathe out, very gently pull in your lower tummy below your belly button – try not to pull in the upper tummy. This muscle works best at 25% of full strength.
- Hold as long as you can, building up to about 30 seconds.
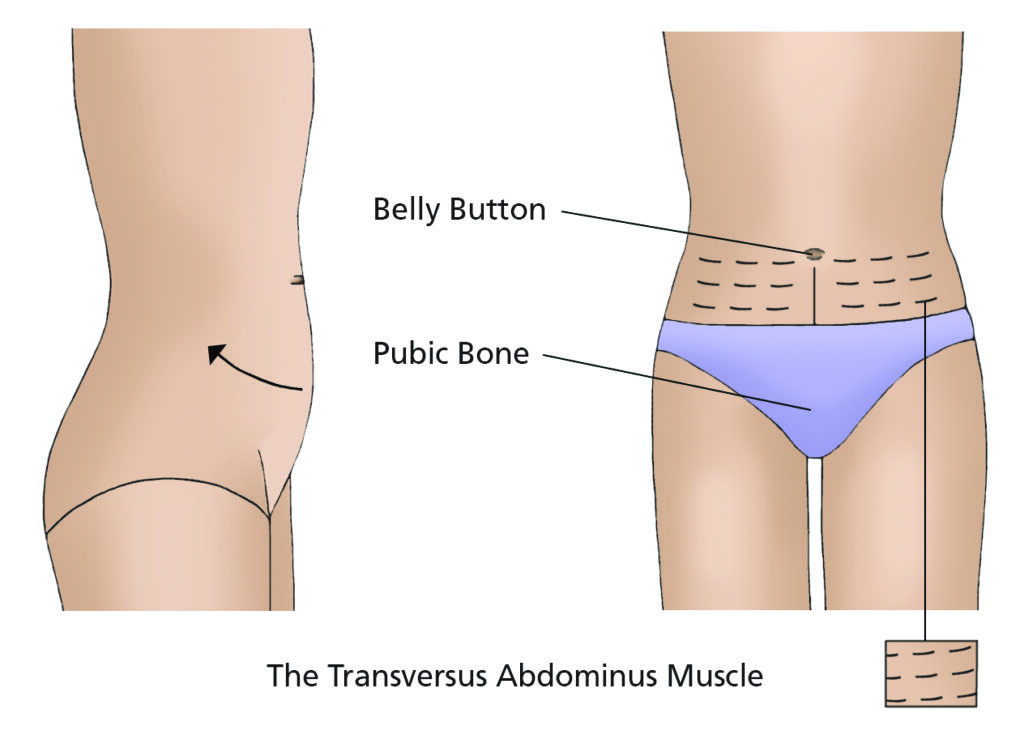
How often should I do the exercises?
Do all three exercises 4-6 times daily for the first month, then 2-3 times daily for the rest of your life. Link to a regular activity or put a sticker somewhere as a reminder.
Using your muscles
- For extra support, tighten up the pelvic floor and deep abdominal muscles before you do anything exertive like coughing or lifting.
- Very gently tighten the pelvic floor muscles for more control if you have difficulty holding on to reach the toilet in time.
- Listen to your body, don’t exercise if it hurts or you are too tired.
Useful Numbers
For queries regarding your admission please call the relevant secretary.
For advice on any medicines you have received from the hospital call:
Gynaecological Cancer Surgery Website
On our website you will find information about our team, what we do, information leaflets and videos.
Visit the Gynaecological Cancer Surgery websiteContacts
For advice please call your Clinical Nurse Specialist (CNS) or Ward J98 (Open 24/7).
If your nurse specialist is not available then please leave a message on the answering machine and they will ring you back. Please note this may not always be the same day. In an EMERGENCY please attend your nearest Accident and Emergency Department.