This information is designed as a general guide to your procedure. If after reading this you have any questions that you feel have not been answered, please contact the relevant Endoscopy department on the numbers below:
Your healthcare professional has recommended that you have a Percutaneous Endoscopic Feeding Tube (PEG) fitted. This leaflet will explain the procedure, how you will need to prepare and what to expect on the day of the procedure. If you have further questions, please ask the doctors or nurses on the ward, your dietitian or you can discuss them with a member of staff on the day of your procedure.
What is a Percutaneous Endoscopic Gastrostomy – PEG?
A PEG is a way of introducing food, fluids and medicines directly into the stomach. A PEG feeding tube is placed between the skin and the stomach. It is inserted by using a flexible tube with a camera on the end (gastroscope). The camera is used to find the best position for the PEG tube. Once in position, the PEG will be secured on the surface of the skin with a fixation device. The procedure takes approximately 20 minutes.
Percutaneous Endoscopic Gastrostomy tube
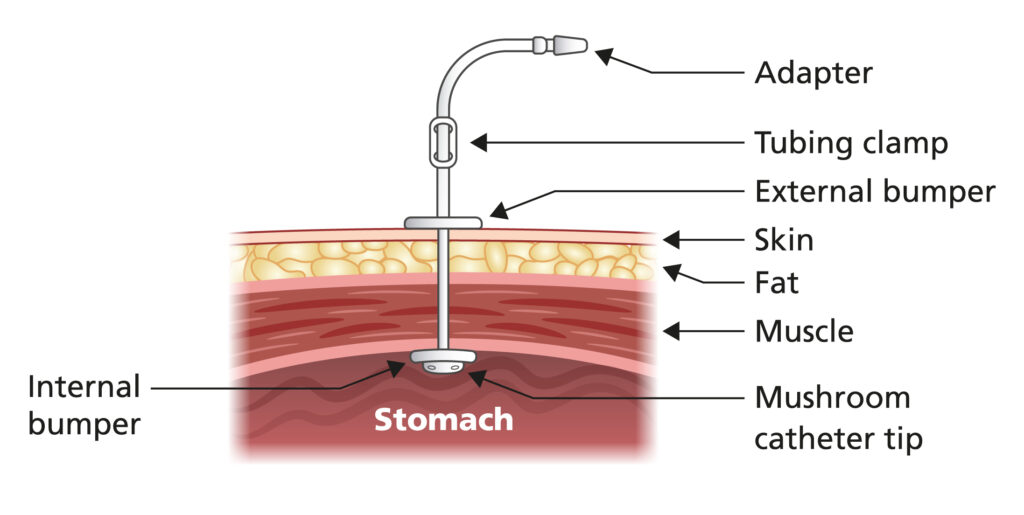
Why am I having a PEG?
There are several reasons why you may not be able to eat normally at the present time. There may be a blockage at the back of your throat or in your gullet (oesophagus), which is preventing food going down normally, or you may have a medical condition or illness which is causing you problems with your swallowing.
Sometimes, your gullet may not be working properly for other reasons. Some patients require a PEG tube for feeding as they are not eating enough to maintain the nutrition their body needs.
A PEG tube bypasses the throat and gullet and is used for people who have difficulty eating and drinking, or if there is a risk of the food going ‘the wrong way’ into the lungs.
Although food and fluids can also be given by passing a thin tube via the nose into the stomach, for people who need tube feeding for long periods of time, a PEG is more comfortable and easier to manage at home. A PEG is a means of providing you with long-term feeding and a balanced diet in order to maintain a good nutritional status.
If you suffer from reflux or regurgitation of food or acid, it is important that you realise that this problem will not be improved by having a PEG.
Also, it is important to remember that PEG feeding will not alter the outcome of your underlying disease or condition.
Back to topWhat are the benefits and alternatives to having a PEG?
A PEG is a safe, reliable and comfortable means of providing nutrition to people who have long-term difficulties swallowing food.
Alternatives include: feeding through a tube placed through the nose into the stomach or inserting a tube directly into the stomach under x-ray control.
There are also other tubes available and some patients choose not to have a feeding tube placed. Speak to your Speech and Language therapist and dietitian about the risks of continuing to eat and drink without a feeding tube.
What are the risks of having a PEG?
The risks associated with your PEG insertion will be discussed with you by the doctor when they discuss the procedure with you. The main risks are detailed below.
It is important that you are aware and understand the risks before you agree to have a PEG tube inserted.
- Having a PEG carries a small risk of a perforation (making a hole) in your oesophagus (gullet) or stomach from the gastroscope. There is also a risk that when the PEG tube is inserted that your bowel could be perforated. If this occurs and there is leakage of stomach or bowel contents, an operation may be necessary to correct it.
- Using sedation can affect your breathing. To reduce this risk, we monitor your pulse and oxygen level.
- Although the PEG tube is inserted using a sterile (aseptic) technique, there is still a risk of infection around the tube site. Before your PEG insertion, you will have specific preparation that will help to reduce the possibility of an infection. If a temporary infection should occur, a course of antibiotics may be necessary.
- A chest infection (also known as pneumonia) can occur after a procedure like this when sedation has been used for the PEG tube insertion.
- You may experience some pain around where the tube has been inserted. If this is persistent, it may be that the fixation device is too tight. This can be easily altered by the ward staff.
- Following the procedure, you may experience a sore throat. This should ease after a few days.
- Other rare complications include damage to loose teeth, crowns or to dental bridgework.
These complications occur in about 20% of cases, and are mostly related to infection around the site of the tube and leakage from around the tube.
A small percentage of patients develop a serious complication, following their PEG insertion. For some patients these complications can be fatal. Patients with complicated medical history are more at risk. Your individual risks will be discussed with you by your doctor.
Back to topWhat preparation will I need?
Most patients are admitted to a ward the day before their PEG insertion. The ward will make sure that you are prepared for your procedure. A PEG insertion must be performed on an empty stomach so that the endoscopist can see the stomach lining clearly. The ward will tell you when to stop eating and drinking. If you are being fed through a tube through your nose, you must not have any fluids passed down this for at least 6 hours.
Do I keep taking my tablets?
You must keep taking any essential tablets. If you are taking any blood thinning tablets, and have not received advice regarding if it is safe to continue, please contact
If you have any questions about if you should stop your medication, please contact the Endoscopy Unit.
What will happen on the day of my procedure?
Before you leave the ward, the nurse taking care of you will ensure that all your preparation has been completed. You will be asked to change into a hospital gown.
When you arrive at the Endoscopy Unit, your personal details will be checked. The assessment nurse will check your medical history and any allergies. You will be able to ask any questions and discuss any worries that you have about the procedure.
Back to topWhat happens in the procedure room?
You will be greeted by two nurses who will remain with you during the procedure. The nurses and the endoscopist will complete a checklist to ensure that all your information is correct. The two endoscopists carrying out the procedure will also be in the procedure room. You will be asked to remove any dentures or glasses and lay on a trolley on your back. Your pulse rate and the oxygen level in your blood are monitored by a probe placed on your finger during the procedure. Before the procedure starts, a plastic mouthpiece is placed between your teeth to keep your mouth slightly open
After you have been given your sedation, the endoscopist will gently pass the endoscope to the back of your tongue and into your stomach, you may gag slightly. This is quite normal and will not interfere with your breathing.
There are known adverse effects from the intravenous drugs administered during the procedure, ranging from mild and common to rare and serious. These include: headaches, nausea, fainting, depression of respiratory and nervous system, which may result in aspiration pneumonia, anaphylaxis and coma. Although these serious complications are rare, they are more common in patients with deeper sedation and / or general anaesthesia.
Saliva and other secretions in your mouth and throat are removed using a suction tube similar to that used by the dentist.
An antiseptic solution will be used to clean the skin on your stomach. A local anaesthetic will be used to numb the area where the PEG tube is to be placed. This may sting initially. Although you will feel some pressure and some prodding over your stomach, you should not feel any pain.
When the endoscopist has decided the best position for your PEG tube with the camera, a small cut will be made in your skin for the PEG tube to pass through. The camera is removed at this point and replaced by the PEG tube. The position of the PEG tube is re-checked so you may be aware of the camera being passed through your mouth on two occasions.
Once in place, a small plastic disc (bumper) inside the stomach stops the tube from falling out. A plastic fixator will be attached to the PEG tube on your stomach and will hold the PEG in position. Sometimes, a small dressing is placed over the tube but this is not always needed. The dressing will be removed in 24 hours.
If you become very uncomfortable, the procedure will be stopped.
PLEASE NOTE:
All hospitals in the trust are teaching hospitals and it may be that a trainee endoscopist performs your procedure under the direct supervision of a consultant, registrar or nurse practitioner.
What happens after the procedure?
You will be transferred to the recovery room after the test. It is likely that your throat will feel sore and in addition, your stomach may feel a little sore and bloated, this should settle after a few days. The doctors on the ward will be able to prescribe some medication for you to help with the discomfort.
Back to top