This leaflet is to give you information about what happens when you need an operation to remove the end of your penis to treat your cancer.
What is a Partial Penectomy?
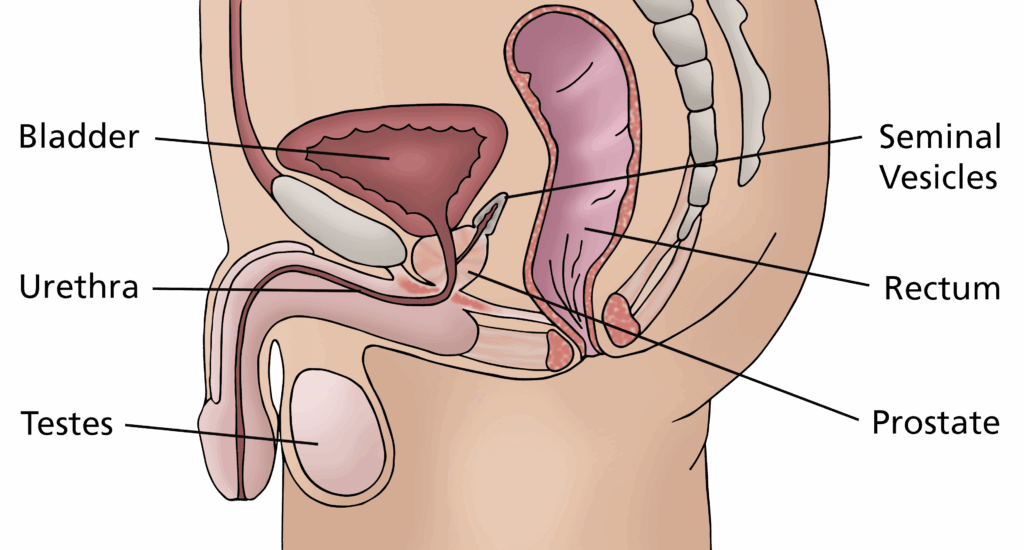
A partial penectomy is an operation to remove the end of your penis where there is a cancer.
The operation will remove the cancer and an additional margin of normal penis to ensure that all of the cancer has been removed.
Why is this necessary?
Your doctor has recommended this treatment to remove the cancer that has grown on your penis.
What are the risks of the operation?
Any surgical intervention can pose some risk. However the majority of patients are unlikely to experience them. The potential risks may include:
- Infection
- Bleeding/ bruising
- Swelling
- Chest infection
- Urinary problems (see below)
- Blood clots in the lower legs (DVT)
- Blood clots in the lungs (PE)
Mobilising around as early as possible will reduce the risk of these. You may be provided with anticoagulation therapy to thin your blood slightly to reduce the risk. You will also be provided with surgical stockings which will promote venous flow, again reducing the risk. You will be required to wear these for your hospital stay.
After the operation you will be able to pass urine but it will likely to spray and you may need to sit down in order to pass urine. Also, you will find it difficult to get an erection and you are likely to find that sexual activity is impossible.
Pre Assessment
Following your clinic appointment you will be placed on a waiting list for surgery. You will be sent a pre-assessment e-form to complete at home. Following this, you may be invited back for tests and to assess your general fitness for the proposed surgery
The day of surgery
On the day of surgery you will be asked to attend the admission lounge where you will be admitted by a nurse, again they will assess your fitness for surgery, record your blood pressure and prepare you for surgery.
You will get the opportunity to be seen by a member of the surgical team performing the surgery (surgeon/anaesthetist) and discuss the procedure again.
Admission times may vary from the time of your surgery. You may be notified by the nursing staff of a potential time of surgery, however this is not definite.
Back to topYour operation
You will be escorted to theatre by a member or the ward staff/theatre staff, regular safety checks will be made when you enter the theatre department and you will proceed to the anaesthetic room.
- The anaesthetist will proceed to administer a general or spinal anaesthetic, depending what is felt to be the best for you.
- During a general anaesthetic you will be asleep for the duration of your procedure.
- For a spinal anaesthetic the anaesthetist will inject medication into your back to ensure you are numb for the duration of the procedure. This can sometime be given with sedation to relax you and make you sleepy.
- The surgeon will then proceed to remove the part of your penis where the cancer has grown; they will also take a margin of normal tissue to ensure the cancer has been fully removed. This will be sent to the laboratory for further testing.
At the end of the operation you will be fitted with a catheter to aid with the healing process.
After your operation
When your surgery is finished you will be taken to the recovery area where you will be monitored until your condition is stable, at this point your nurse will be called to escort you back to the ward (this may be a different ward to the one you were admitted to).
Painkillers will be offered to you on a regular basis as it is important that you feel as comfortable as possible after the operation.
The dressing on the penis, which is put on in the operating theatre, is usually removed a day or two after the operation. The catheter draining urine from your bladder will be taken out 48 hours after the operation and the ward will assess that you are passing urine with no problems before discharge.
Discharge Preparation
The ward staff will check your wound regularly, alongside the doctors who will do regular ward round to assess your progress. Once each member of the multidisciplinary team is happy you will be allowed to go home.
We will give you pain killers to take home with you and we would advise you to take them as they have been prescribed for you. Please do not exceed the stated dose on the pack. Generally, the discomfort will take a few weeks to go away. You may also receive antibiotic therapy prophylactically to minimise the risk of infection.
The stitches used in the operation are often dissolvable and will fall out over time – usually within a month.
How will you recover?
Due to the nature of the operation the end of your urethra (water passage) has been cut away, once the catheter is removed your flow of urine is likely to have altered and is likely to spray, this is normal.
It may be necessary for you to pass urine in a seated position, alternately if this becomes bothersome a funnel device is available on prescription. (This can be placed over the penis when urinating and it directs the spray. It is washable and can be taken anywhere. If this is a problem for you your urology nurse specialist will provide you with the relevant details/support).The appearance of your penis will change, often looking shorter, depending on the size of the tumour. The sensation to the tip of your penis will be altered and it is can affect your sexual function.
It is likely that you will still able to get an erection after the operation, however this may not always be the case. This can be distressing and may take time to come to terms with. It is advised to discuss this with your partner/ close family member or you may find it useful to contact a counsellor/Clinical Nurse Specialist.
Back to topFollow up appointment
Following your surgery you may be asked to return to be seen by the nurse specialist to review your wound 7-10 days post op. This is to ensure your wound is healing as expected.
You will later be seen by a consultant to discuss your progress and the results of your histology in the outpatient clinic 4-6 weeks after you go home.
If you have any problems or worries before then you can ring the nurse specialist. There is an answerphone service, please leave a message with your name and telephone number and your call will be returned at the earliest convenience. Alternatively you can ring your consultant’s secretary.
Contact us:
Urology Clinical Nurse Specialist
Leeds Cancer Support
Leeds Cancer Support complements care provided by your clinical team. We offer access to information and a wide range of support, in a welcoming environment for you, your family and friends.
We can be found in the information lounges in Bexley Wing and also in the purpose built Robert Ogden Macmillan Centre.
The Sir Robert Ogden Macmillan Centre
The Centre is on the St James’s Hospital site and offers a variety of support services including counselling, support groups and complementary therapies. These therapies include Reiki, relaxation and visualisation, hand and foot massage and many others. You can just drop in for a coffee and a chat anytime. Open from 10:00am – 4:00pm Monday to Friday.
Back to topHealth Talk support service
Health talk is an online service where you can find information and support by seeing and hearing patients real life experiences.
In co-ordination with researchers from the Centre for Men’s Health at Leeds Metropolitan University spoke to 27 men in their own homes. You can explore what these people felt about issues such as symptoms, treatment, body image and sex. We hope you find the information helpful and reassuring.
www.healthtalk.orgContact numbers for Leeds Cancer Support
All the above services can be emailed via the link below.
Leeds Cancer SupportWhere can I find more Information?
References
- Orchid male cancer support 2017. Partial Penectomy
- Orchid male cancer support 2017. Total Penectomy
- The Christie Patient Information Service May 2015. CHR/SUR/600/17.06.08 version 4
