You will be given a separate leaflet called ‘Gynaecological Oncology Surgery – Enhanced Recovery Programme’ which will explain about what to expect when you come in for your surgery and advice for recovery at home.
If you have recently been diagnosed with cancer of the cervix, you may find that you are experiencing a wide range of emotions. These can include fear, anger, denial, low mood and anxiety. Reactions differ from one person to another and there is no right or wrong way to feel. Whatever you may be feeling at present, try talking about it with someone who can help; such as your consultant, gynaecology specialist nurse or GP. They will listen to you and answer any questions that you may have. They can also put you in touch with other professionals or support organisations if you wish. Some useful contact numbers are listed at the back of this booklet.
There are two types of surgery that can be used to treat cervical cancer – trachelectomy or radical hysterectomy.
What is a Trachelectomy?
A trachelectomy is an operation for early stage cervical cancer that preserves fertility for women who still wish to have children. The procedure involves the removal of the cervix (neck of the womb), tissue around the cervix (parametrial tissue) and a small section of the upper part of the vagina.
A large permanent stitch is inserted around the opening to the uterus (womb), which is strong enough to support a future pregnancy but still allows you to have your monthly period and to conceive. The uterus (womb) ovaries and tubes are left in place. A sample of pelvic lymph nodes are taken because the cancer can spread to these nodes (see diagram). These nodes will be tested to see if they contain any cancer cells. You will have a general anaesthetic and so will be asleep during the operation.
Who is suitable for Trachelectomy?
The cancer must be small and confined to the cervix for you to be considered for this operation and you must have a strong desire to preserve your potential fertility. A careful assessment will be carried out, after which the surgeon will discuss with you all aspects of the operation and the implications for possible future pregnancies.
Your ovaries will continue to produce eggs and you will still have a period each month. If you discover you are pregnant, you will need to contact your GP as you will be referred to an obstetrician and hospital with neonatal facilities. You will also need a caesarean section delivery.
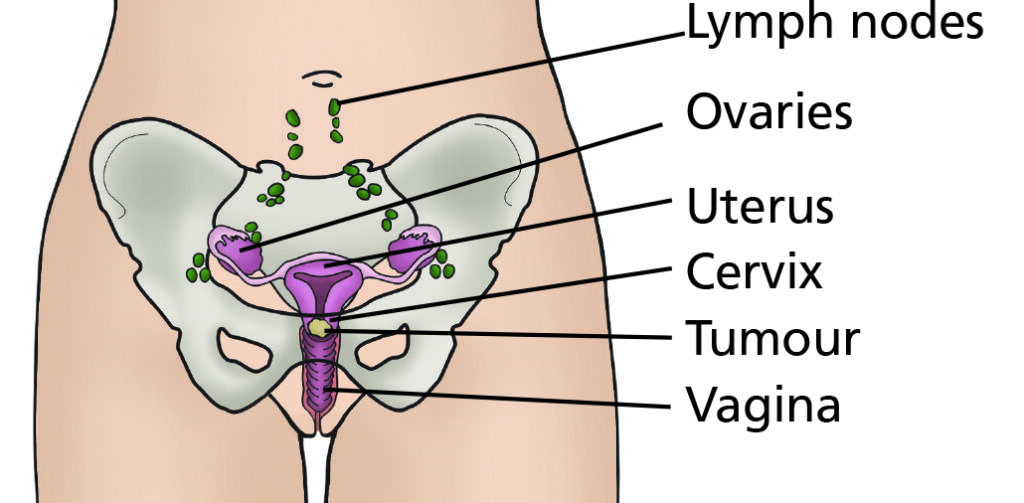
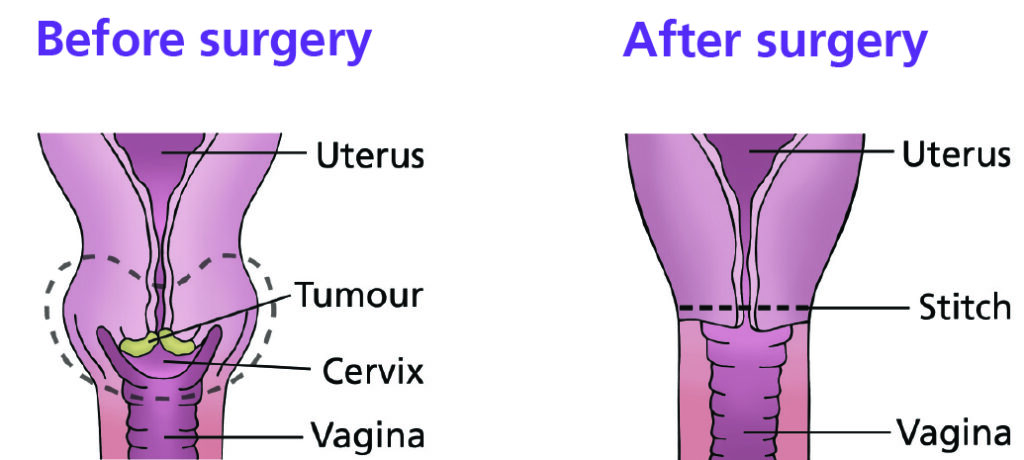
These diagrams show where the large permanent stitch is inserted around the opening to the uterus (womb) which is strong enough to support a future pregnancy but still allows you to have your monthly period and to conceive.
What is a Radical Hysterectomy?
A radical hysterectomy (sometimes called a Wertheim’s hysterectomy) may be recommended if the cancer is confined to the cervix, and you do not have a strong desire to preserve your fertility. It involves removing the uterus (womb), cervix (neck of the womb), tissue around the cervix (parametrial tissue), fallopian tubes, the upper part of the vagina, pelvic lymph nodes and sometimes the ovaries. You will have a general anaesthetic, which means you will be asleep for the entire operation. The aim of the operation is to remove all of the cancer. If there is evidence that the cancer has spread, you may be offered further treatment such as radiotherapy or chemotherapy. This will be discussed with you when all of your results are available.
Will I have a scar?
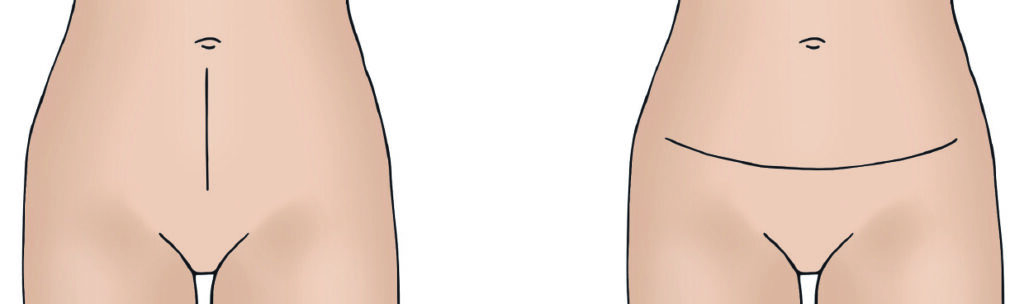
For both trachelectomy and radical hysterectomy, the cut will be made either across your tummy, just above your pubic hair, or vertically (up and down). The wound will be closed using either stitches or clips.
Most patients have dissolvable stitches. You will have a scar, but it will become less noticeable over time. The area around the scar will feel numb for a while after the operation but sensation will usually return to it.
Incision Types
What are the risks of surgery?
All surgery carries some risks and your surgeon will explain the risks to you before you sign your consent form. This form confirms that you agree to have the operation and understand what it involves.
Possible risks and complications are:
- Problems caused by having a general anaesthetic – for example, you may feel sick afterwards. It is also possible to have an allergic reaction, although this is rare. Please tell your doctor about any allergies you have.
- Heavy bleeding during or after the operation; this may need to be treated with a blood transfusion.
- Infection; this would be treated with antibiotics.
- Damage to your bowel, bladder or ureters (the tubes that carry urine from the kidneys to the bladder) during surgery – this would be repaired during your operation.
- A blood clot in the leg (deep vein thrombosis) which can sometimes lead to a blood clot in the lungs (pulmonary embolus) – moving around as soon as possible after your operation can help to prevent this. You will be given surgical stockings (known as TEDS) to wear and injections to thin the blood which both help to reduce the risk of blood clots. You may continue to have these injections for up to four weeks.
- Incisional hernia; a weakness in the wound, allowing tissue or bowel to push through and appear like a bulge. Incisional hernias can develop months or years after surgery and are repaired by another operation.
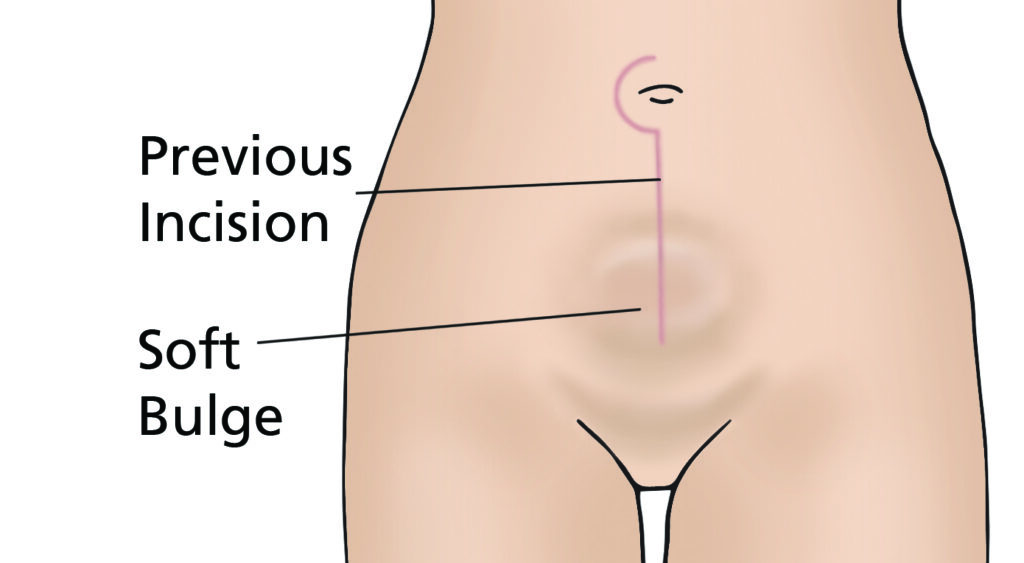
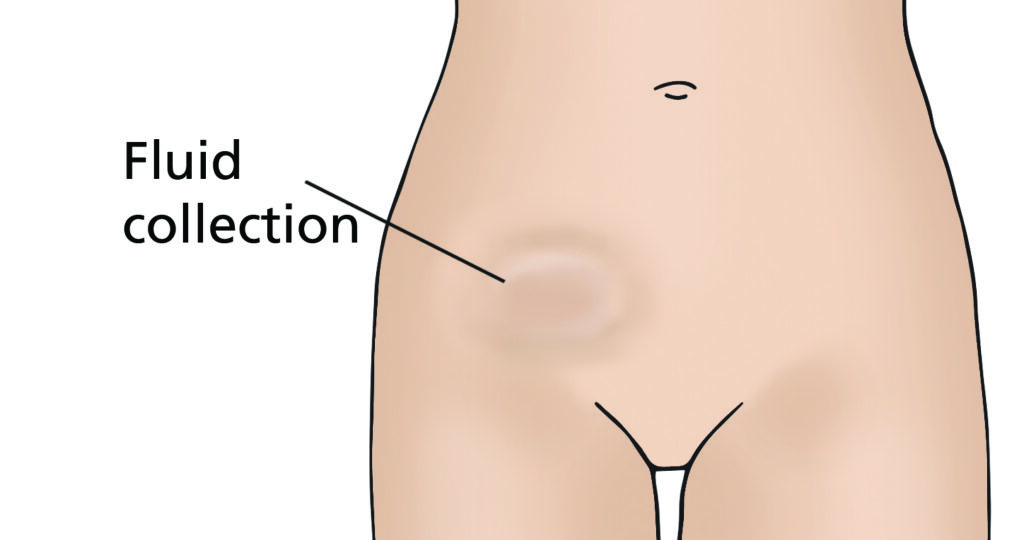
- Lymphocyst; this is a fluid collection at the site where lymph nodes have been removed. The fluid is often naturally reabsorbed by your body but may require draining if large or causing you discomfort.
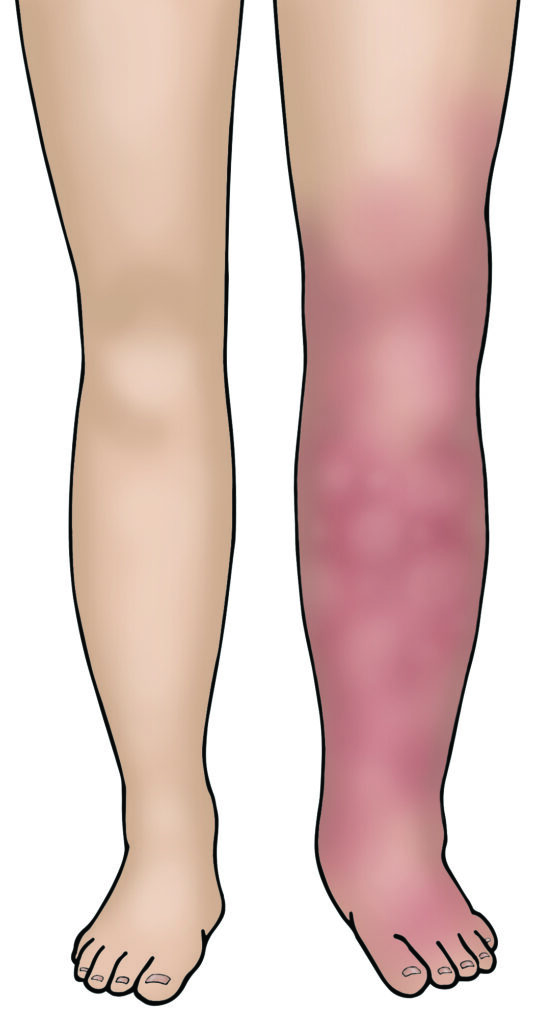
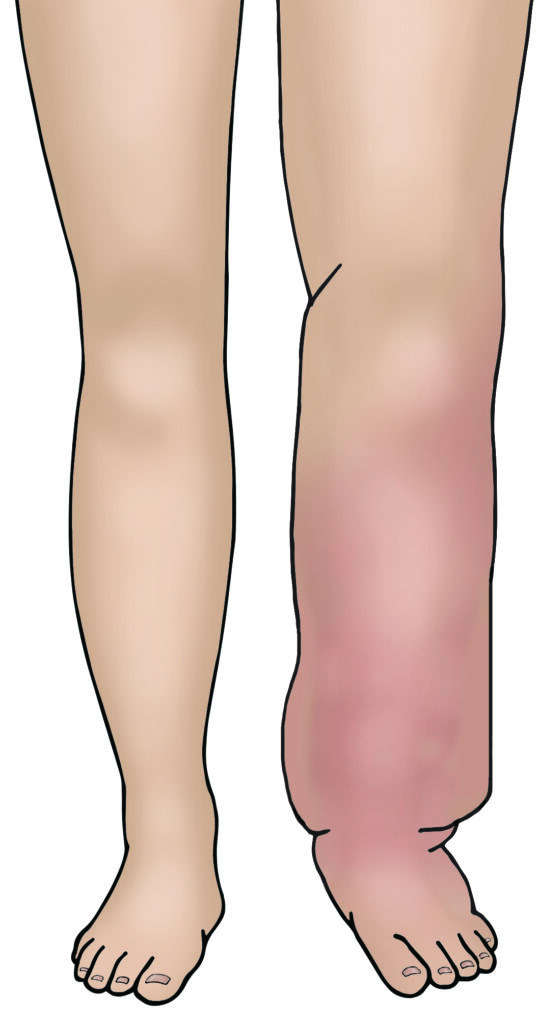
- Lymphoedema; if you have some lymph nodes removed during surgery there is a small risk that in the future your body will find it harder to drain fluid from your legs and lower body. This causes swelling of the legs and lower body known as lymphoedema. If you develop this problem then you can be treated by a lymphoedema specialist. You can discuss this further with your gynaecology specialist nurse or doctor. There is also a booklet you can read that can give you more information.
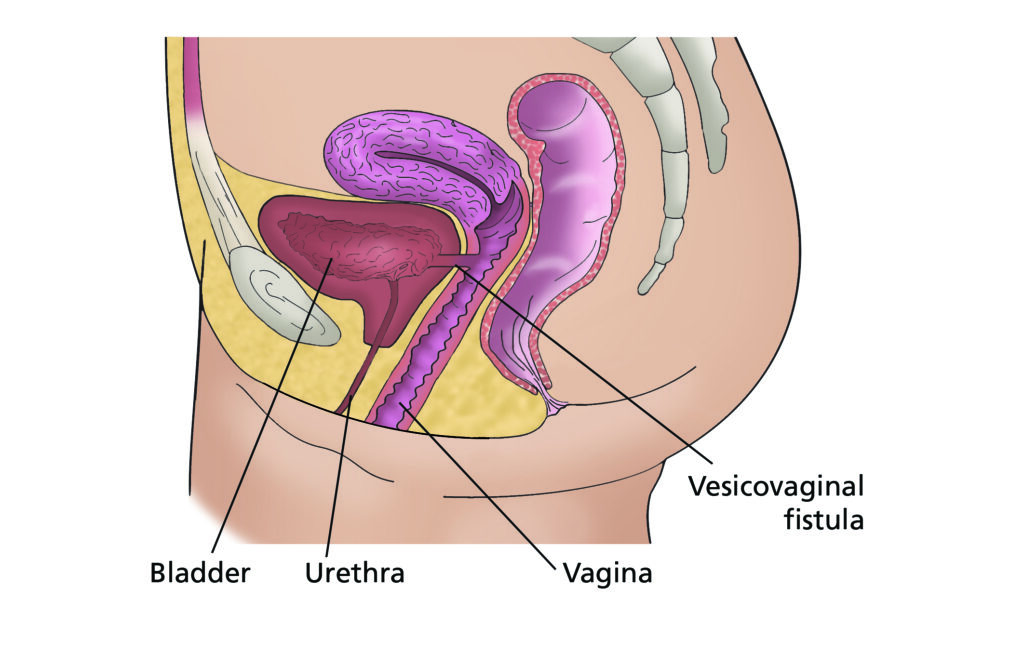
- A vesicovaginal fistula is a hole between the bladder and vagina. It allows urine to pass from the bladder to the vagina.
- A rectovaginal fistula is a hole between the rectum and the vagina. It allows faeces to pass from the rectum to the vagina.
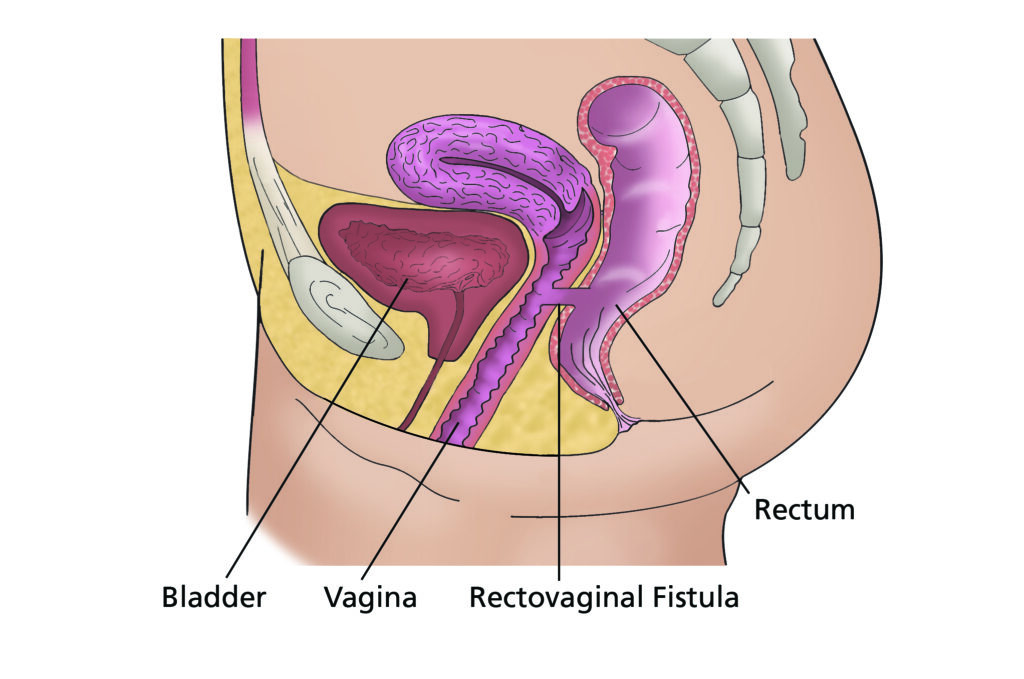
- Fistulas can be repaired but sometimes it will involve another operation.
- You have an increased risk of urinary retention. You will have a catheter (fine tube) in your bladder to drain urine and this will usually be removed 4-7 days after your operation depending on your surgeon wishes. If your catheter is to remain in for seven days then you can usually go home and return a few days later to have it removed.
- You may experience some numbness at the tops of your legs or the inside of your thighs after your operation. This usually improves over time but occasionally there may be some permanent altered sensation.
What else may happen as a result of surgery?
Your bladder may take some time to begin working properly again. Some women have a loss of feeling in their bladder and therefore do not know when their bladder is full. This may take some time to return to normal. During this time you need to go to the toilet regularly to empty your bladder. Some women find that their urine stream is slower so it may take longer to pass urine. This usually improves as your body recovers from surgery. Rocking gently backwards and forwards or side to side whilst sat on the toilet can help to fully empty your bladder.
Your bowels may take some time to begin working properly again. Some women have a sluggish bowel for a number of days after surgery which can cause you to feel sick until it starts to work again. If this happens then you will be advised to walk around the ward as much as possible to stimulate your bowels to work. This can be difficult if you are feeling unwell but it is important to do so to speed up your recovery. We will also give you anti-sickness medication. Passing wind is a good sign that your bowels are starting to work.
Trapped wind and wind pain is very common after surgery. Walking around as much as possible can help relieve this. You may find that peppermint tea and/or peppermint capsules helpful which are both available on the ward. Wind usually starts to improve once you are having your bowels opened.
Loss of fertility after hysterectomy
At any age, having your ovaries and/or womb removed can affect the way you feel about yourself. A hysterectomy will prevent you from getting pregnant. The loss of fertility can have a huge impact on you if you have not yet started or completed your family and you have an operation that takes that choice away. You may want to make sure that you have explored all your options. It is important that you have the opportunity to discuss this and your feelings with your specialist nurse before your operation. They will continue to offer you support when you are recovering from the operation. Advice is also available from our specialist fertility team.
Will I need hormone replacement therapy (HRT)?
The use of HRT for women who have been diagnosed with a gynaecological cancer is not straightforward. A number of different factors influence whether or not HRT is recommended. Please discuss the options available to you with your consultant or specialist nurse.
Should I continue to have cervical smears?
No. The cervix has been removed and therefore smears are not required.
Will I need further treatment?
You will not usually require further treatment if the tissue analysis shows the pelvic lymph nodes are negative for cancer and all the cancer tissue has been removed. However, if the cancer has not been fully removed or if cancer is found in your lymph nodes then you may require radiotherapy or possibly chemotherapy. The appropriate team will discuss this with you if necessary.
Is it normal to feel weepy or depressed afterwards?
Yes. It is a very common reaction to the operation. If these feelings persist when you leave the hospital, you may wish to discuss them with your GP or specialist nurse. There are also local and national support groups that you can contact. Details are given at the end of this booklet.
When can I go home?
You will usually be able to go home roughly 3-5 days after your operation. This depends on your individual recovery, how you feel physically and emotionally and the support available at home. If you require hospital transport for your discharge home, please let a member of staff know well in advance.
Will I need to visit the hospital again after my operation?
Yes. It is very important that you attend any further appointments arranged either at St James’s Hospital, Leeds or at the hospital that referred you for your treatment. The tissue results (histology) from your surgery can take about
3-4 weeks to return.
An appointment for the outpatient clinic will be made to discuss these results with you and if any further treatment is necessary.
Useful Numbers
For queries regarding your admission please call the relevant secretary.
For advice on any medicines you have received from the hospital call:
Gynaecological Cancer Surgery Website
On our website you will find information about our team, what we do, information leaflets and videos.
Visit the Gynaecological Cancer Surgery websiteContacts
For advice please call your Clinical Nurse Specialist (CNS) or Ward J98 (Open 24/7).
If your nurse specialist is not available then please leave a message on the answering machine and they will ring you back. Please note this may not always be the same day. In an EMERGENCY please attend your nearest Accident and Emergency Department.