What is carotid artery stenting?
Carotid artery stenting (CAS) is a minimally invasive procedure used to treat narrowing of the carotid artery in the neck. The carotid arteries supply blood to the brain. Narrowing (stenosis) is usually caused by atherosclerosis (fatty plaque). CAS aims to reduce the risk of stroke by widening the artery with a stent.
How do I prepare?
You have been referred to Interventional Radiology by your vascular surgeon or stroke physician, who has already assessed you. The interventional radiologist will usually contact you by telephone and will either arrange to see you in clinic or review you on the ward before the procedure, depending on urgency. You will need antiplatelet medication. This is often aspirin plus clopidogrel for a period before and after the procedure (follow your doctor’s instructions). You will be admitted to a ward either the night before or the morning of the procedure. Please bring a list of your medications.
If you take anticoagulant (blood-thinning) medicines (e.g. warfarin or apixaban), please ensure you have been given instructions about stopping them before your procedure. If not, contact us urgently, as the procedure may have to be cancelled. You should continue taking all your usual medicines (e.g. for blood pressure or diabetes) unless you have been advised otherwise.
Fasting prior to the procedure may be necessary. You will receive specific instructions.
How is it performed?
Consent
Before the procedure, the interventional radiologist will meet you in our recovery area to discuss why we are doing the procedure and the risks. This is where you give your consent. This is a good opportunity to ask any questions you might have about the procedure.
Anaesthetic
The procedure is usually performed under local anaesthetic with sedation if required. The skin in the groin will be cleaned with antiseptic, draped with sterile towels and numbed with local anaesthetic. This stings a little. You will also be connected to equipment to monitor your heart beat and blood pressure.
Operation
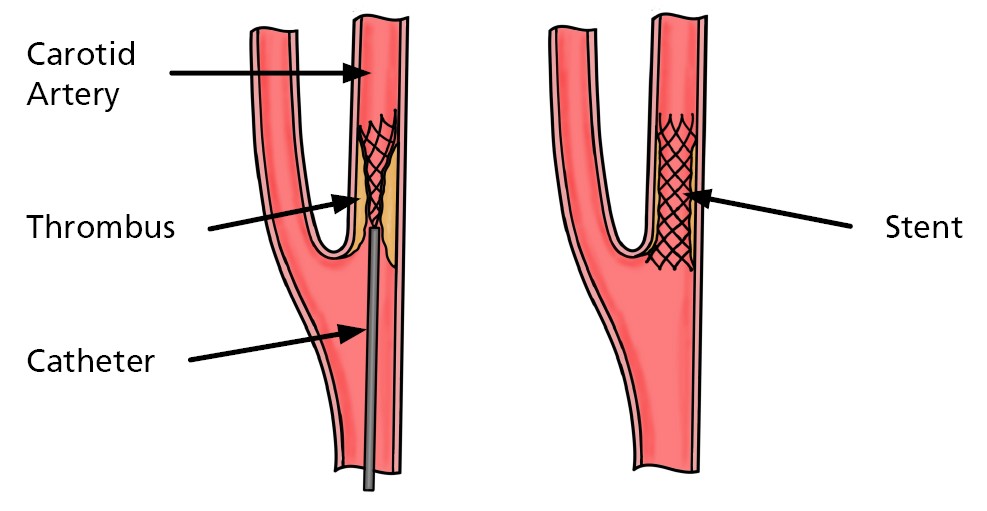
The procedure typically takes about 60 – 120 minutes, though every patient is different and some operations may take longer. A small tube (catheter) is inserted into an artery at the groin. Contrast dye is injected and X ray imaging is used to guide the catheter to the carotid artery. A cerebral protection device (filter) may be used to reduce the risk of debris travelling to the brain. A balloon may be inflated to widen the narrowing (angioplasty). A stent (metal mesh tube) is deployed to keep the artery open; further balloon inflation may be needed. You will be monitored closely during and after the procedure. Blood pressure and heart rate changes can occur and are treated promptly.
Staff Involved
Interventional Radiology (IR) procedures are performed by a multidisciplinary team. The team includes the following key Staff:
- Interventional Radiologist (Consultant/Fellow): A doctor specially trained in minimally invasive, image-guided techniques who performs the procedure.
- Radiology Nurses: Highly trained nurses who care for the patient before, during, and after the procedure. They assist with sedation, monitor vital signs (heart rate, breathing, oxygen levels), and may “scrub in” to assist the radiologist directly.
- Radiographers: Experts in imaging equipment who operate the machines to provide real-time guidance for the doctor.
- Senior Clinical Support Workers (SCSWs): Assist with the setup of the room, patient positioning, and maintenance of sterile conditions.
What are the risks?
Your doctor will discuss risks relevant to you. The main purpose of CAS is to reduce the long‑term risk of stroke, but the procedure itself carries a small risk of stroke (around 3%).
Common/expected effects:
- Bruising or discomfort at the puncture site.
- Headache or neck discomfort for a short time.
- Temporary changes in blood pressure or heart rate.
Serious risks (uncommon but important):
- Stroke or transient ischaemic attack (TIA) during or shortly after the procedure.
- Bleeding requiring transfusion or further procedure.
- Artery damage/dissection, blockage, or need for emergency surgery.
- Allergic reaction to contrast dye.
- Kidney injury from contrast dye (especially if you have kidney disease).
- Heart complications such as heart attack or abnormal rhythm.
- Infection (rare).
- Death (very rare).
X-rays will be used to make images of your body and guide your doctor during the procedure. X-rays are a type of radiation. We are all exposed to low levels of natural radiation as part of our everyday lives and medical x-rays give an extra dose of radiation. Radiation can increase your chances of developing cancer many years or decades after the exposure. The chances of this happening to you as a result of this procedure are considered to be very low.
In some very rare situations, you might experience some hair loss or some reddening of the skin in the area that was treated. If this happens, you should contact your clinical team who will be able to give some advice on the simple steps you can take to look after your skin.
It is important to remember that your doctor thinks that the benefits of this procedure outweigh any risks from the radiation. We will make sure that the amount of radiation used in your procedure is as low as possible.
What to expect from this procedure?
Admission
You will attend the Radiology Theatres department on the morning of the procedure. You will have a cannula (a small plastic tube in the vein) to allow us to give any medication or fluid intravenously if required. You will be kept in hospital for observation overnight in a ward.
Recovery
After the procedure you will be monitored in recovery and then usually on a ward overnight. Neurological observations will be performed regularly. You will need bed rest for at least two hours. If you have any pain or discomfort in your neck, you’ll be given painkillers as prescribed.
Aftercare
You will be closely monitored for a few hours after the procedure to ensure there are no immediate complications. If there are no complications, you will be allowed to go home the following day. You will need to take medications to prevent a blood clot from forming within the stent. One of these medications will need to be taken for your rest of your life.
Care at Home
The following advice will support your recovery:
- Exercise – gradual return to exercise is best, focusing on light activity initially and avoiding heavy lifting/strenuous activity for 5 – 7 days.
- Work – You may be able to go back to work after a few weeks, but it will depend on the type of work you do.
- Driving: you may have driving restrictions after TIA/stroke or after vascular procedures. Follow DVLA/medical advice before driving.
- Medicines: continue antiplatelet tablets and other medications as prescribed. Do not stop these without medical advice.
- Follow-up – You may have a follow-up appointment with your specialist after your operation to check on your progress and discuss any problems you have. A scan is usually scheduled four to six weeks after the procedure to check the stent.
- Puncture site: keep clean and dry; mild bruising is common. Seek help if there is swelling, severe pain or bleeding.
- Seek urgent medical attention if you develop new weakness, speech/vision disturbance, severe headache, or collapse.
Results
CAS can reduce the risk of stroke in selected patients with significant carotid stenosis. Long‑term success depends on controlling vascular risk factors and taking prescribed medication. Follow‑up ultrasound may be arranged to check the stent and further procedures may be necessary to ensure the stent functions optimally. Please seek urgent medical attention if you develop neurological symptoms such as sudden weakness, numbness, facial droop, speech difficulty, or loss of vision.
Contact information
We hope some of your questions have been answered by this leaflet. If there are any questions you would like to ask before you come for your operation, please get in touch.
Via telephone:
Interventional Radiology SJUH: 0113 206 6841
(Monday – Friday from 9am until 5pm, except Bank Holidays)
Interventional Radiology LGI: 0113 392 3311
(Monday – Friday from 9am until 5pm, except Bank Holidays)
Your GP or NHS direct on 111
Call 999 for life-threatening emergency
Or via email: [email protected]
How to get to our department
We are located in the Lincoln Wing of SJUH, Ground Floor. Check this link to see how to get to us AccessAble – Your Accessibility Guide.
www.accessable.co.uk/leeds-teaching-hospitals-nhs-trust/st-james-s-university-hospital/access-guides/lincoln-wing
We are located in the Jubilee Wing of LGI, Ground Floor. Check this link to see how to get to us AccessAble – Your Accessibility Guide.
www.accessable.co.uk/leeds-teaching-hospitals-nhs-trust/leeds-general-infirmary/access-guides/jubilee-wing