If you have any questions or concerns, or would like any further information, please ask your dentist.
‘Endodontic treatment’ refers to a range of procedures used to treat or prevent an infection inside your tooth, particularly within the root canals.
During the procedure, the area around the affected tooth will be numbed using local anaesthetic injections. You will remain awake throughout the treatment and can return home shortly after it is completed.
Why might I need root canal treatment?
Healthy teeth have a crown and a root. The crown is the white part, which is visible in the mouth and the root is the part underneath the gum surrounded by bone. Each root has a narrow tube inside it which is called a ‘root canal’ or ‘pulp’, which contains the nerve and blood supply to the tooth.
When a tooth is injured, the dental pulp can die. Bacteria can enter this space in the root and cause pain and/or infection (abscesses, gum boils and cysts). RCT is carried out to treat or prevent this pain and an infection inside your tooth, and try to save the tooth.
Why might root canal treatment be needed?
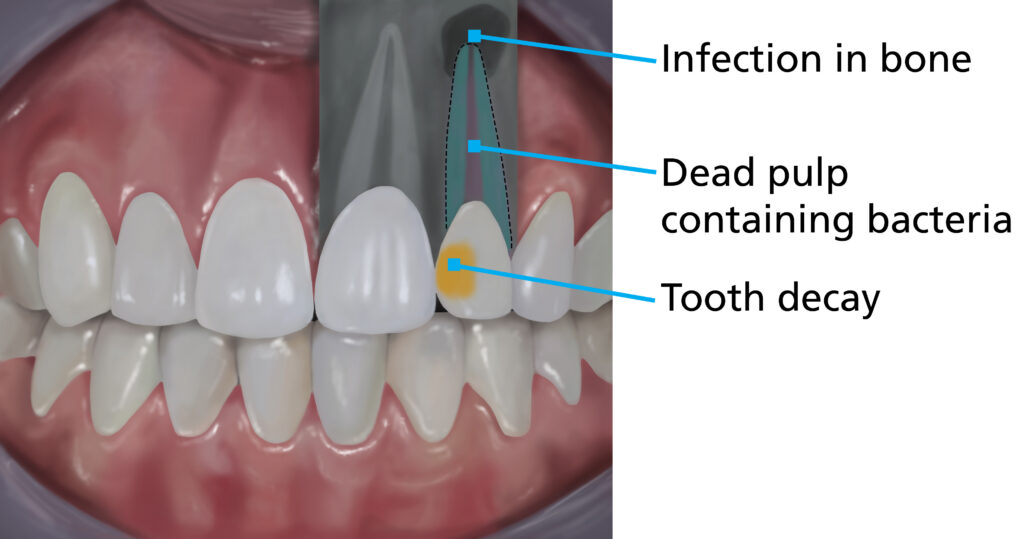
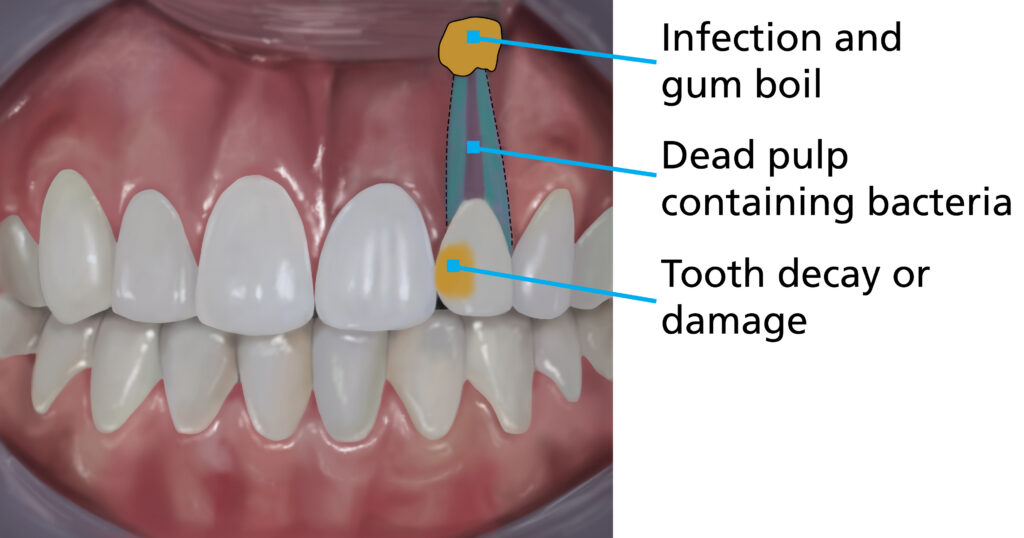
What happens if I don’t have root canal treatment?
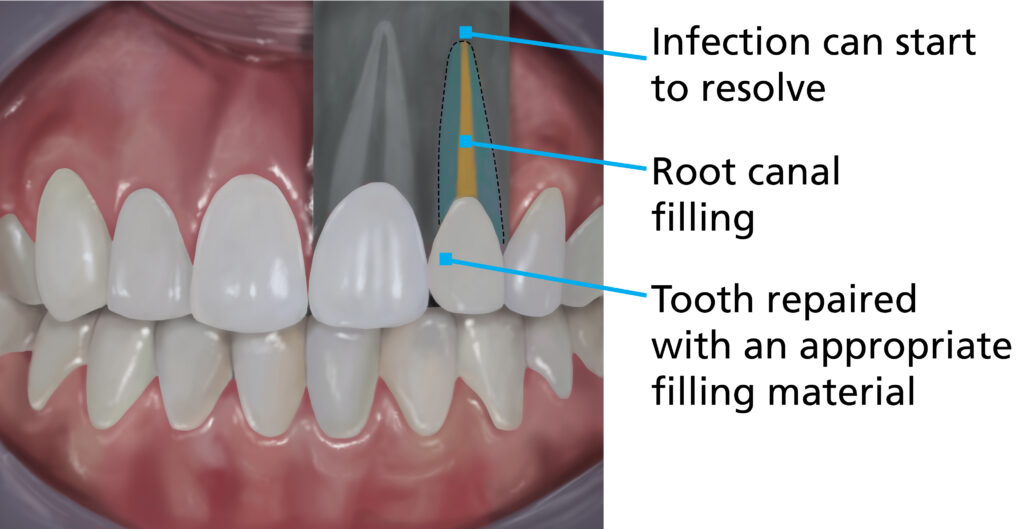
Tooth after successful root canal treatment
You might need this treatment if you have:
- Extensive decay.
- A deep, fractured, or leaky filling or crown.
- Repeated replacement of fillings.
- Extensive gum disease and its treatment.
- Tooth injuries.
- A tooth that has developed a crack.
Why might I need re-root canal treatment?
Re-root canal treatment is undertaken when a previous root canal treatment has failed or is considered unsatisfactory. Reasons for failure can include:
- Persistent infection.
- Re-infection from a leaky filling, crown, or decay.
- The presence of cracks or fractures.
- The presence of a cyst around the root end.
Sometimes, Re-RCT is also performed to improve the technical quality of a root filling before a new crown or bridge, or if a dental implant is planned nearby.
How successful is endodontic treatment?
RCT is a very common and highly successful procedure:
- The success rate is about 96% when there is no inflammation at the root end.
- With existing inflammation, the success rate is about 85%.
- While highly successful, results cannot be guaranteed, as success depends on your body eliminating the infection after the tooth is disinfected and filled.
- In a small number of cases, persistent infections can lead to failure, and further treatment like re-treatment or root tip surgery may be considered.
For Re-RCT, success rates range from 40% to 80% depending on the initial problem. Persistent infection is possible, and if treatment fails, surgery or extraction will be needed. No guarantee of success can be offered.
On the day of your endodontic treatment
On the day of your treatment, it is important to eat as normal beforehand. Take any medications, including painkillers, as normal- unless your dentist or doctor has specifically told you otherwise.
At your appointment, the team will introduce themselves to you. There will be three or four people in the room. Your dentist will explain the treatment to you, and check that you are still happy to go ahead.
What is involved in endodontic treatment?
The treatment involves several steps:
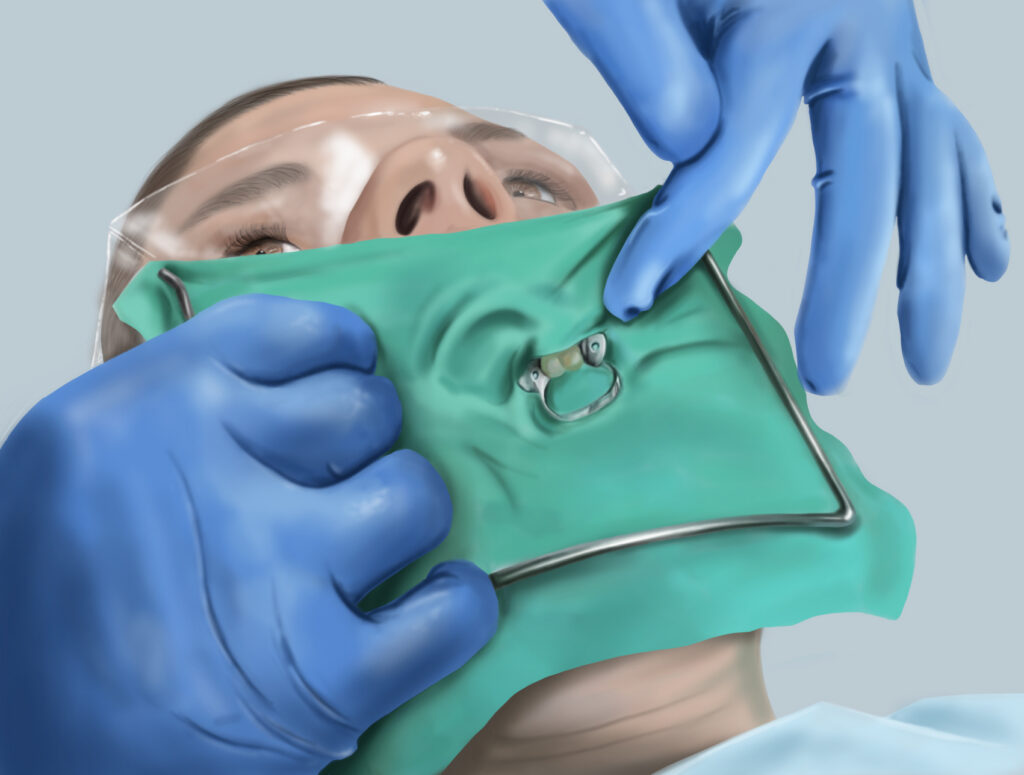
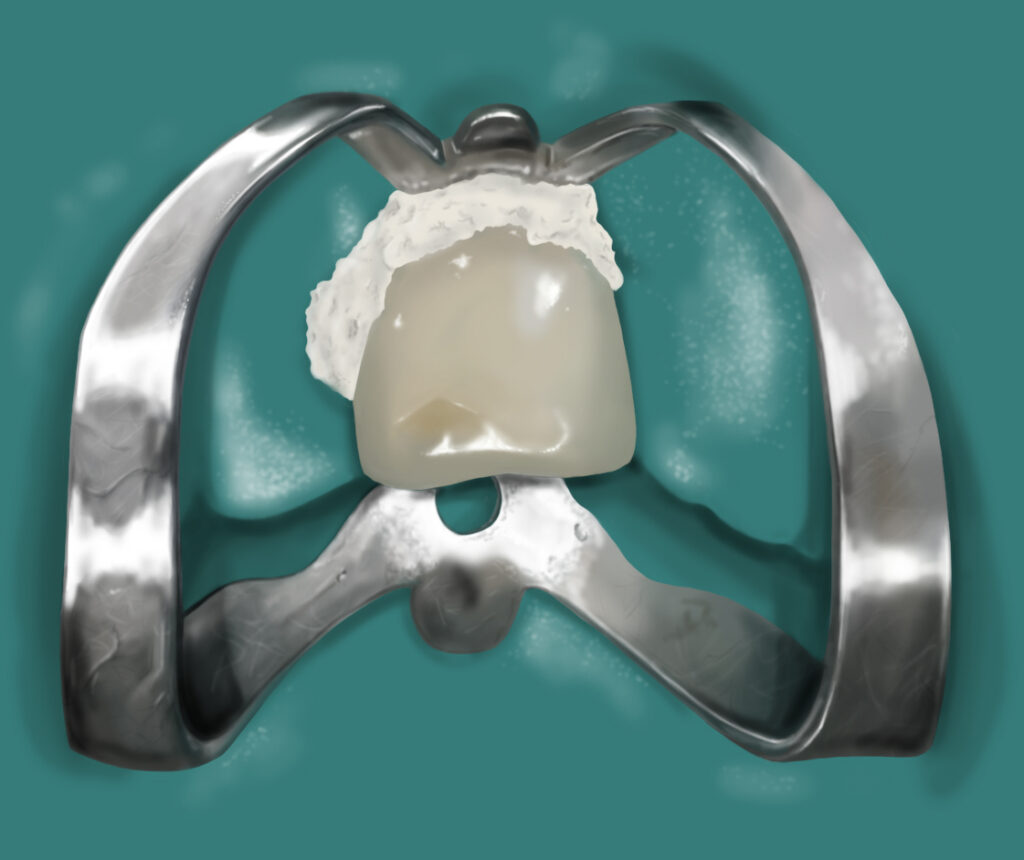
- Placement of a ‘rubber dam’ (‘raincoat’ isolation) – This keeps the tooth dry and prevents infection from saliva.
- Entry to the root canals – This is done by drilling through the tooth, an existing filling, or a crown (which might need temporary replacement) to create a small window to allow access to the root canal inside.
- Preparation of root canals – Specialised instruments are used to prepare the root canals for disinfection, often with the aid of a microscope.
- X-rays – X-rays are taken to check the length of the canals and the quality of the filling.
- Disinfection – dental bleach is used to wash the root canals.
- Temporary dressing – If more than one appointment is needed, the tooth will be temporarily dressed.
- Root filling – A root filling is placed to prevent re-infection.
- Final restoration – A new filling, crown, or onlay will likely be needed after the RCT or Re-RCT is completed. This is usually provided by your own dentist, and the success of the treatment depends on this final seal.
For Re-RCT, the treatment usually involves removal of previous root filling material.
Will I experience pain during treatment?
Generally, no, pain during treatment is rare. The treatment is performed under local anaesthetic (‘numbing injections’).
- If the nerve is very inflamed, local anaesthetic may be less effective, but strategies are available to manage this.
- Your tooth may feel sore after treatment for 3-4 days, and sometimes longer, which can be managed with painkillers like ibuprofen and paracetamol.
- About 1-5% of people may experience a flare-up with increasing pain or swelling 3-4 days later, which might require antibiotics.
How long does the treatment usually take?
- Appointments may typically last 1 ½ – 2 hours.
- More than one appointment may be necessary for complex teeth or heavily infected teeth.
- The process requires skill, time, and patience.
- Feel free to bring headphones for comfort.
Is root canal treatment always possible?
Sometimes, a full diagnosis is only possible after opening the tooth.
- If there isn’t enough tooth structure left, extraction may be necessary. In such cases, replacement options will be discussed, and you will be referred back to your dentist.
- Root canal treatment may also be impossible if there are blockages, curves, or an inability to find the canal.
- For Re-RCT, feasibility also depends on the quality of the previous treatment and the reason for its failure. Problems like broken instruments, perforations (extra openings), or blocked canals from previous treatment can make further treatment much harder. If a certain standard cannot be achieved, extraction may be advised.
What are the risks associated with root canal treatment?
All treatment has risks. You will be given advice on how to look after yourself afterwards to reduce these risks.
The most common risks of root canal treatment include:
- Mild discomfort after treatment, rarely pain during treatment.
- Incomplete healing, which might require further procedures like root-tip surgery, re-treatment, or tooth removal.
- Failure to find and negotiate the root canal or canals, or to remove old root filling material.
- Blockage of root canals.
- Fracture of files in the canal.
- Fracture, chipping, or loosening of an existing crown or veneer.
- Tooth/root perforation (extra openings) of the tooth/canals with instruments.
- Leakage of dental bleach into the mouth.
- Extrusion of dental bleach or filling through the root end: This may cause pain, burning, swelling, bruising, numbness, and/or tingling of the face, and may require further treatment.
- Risk of tooth or root fracture afterwards, as the tooth may be weaker.
- Flare-up of infection between appointments (1-5% of people) – this may present as pain or swelling and might require antibiotics. Should this occur, please refer to the contact details below for how to contact us in an emergency.
What happens after my root canal treatment?
After completion of your root canal treatment, you will need to return to your own dentist for a final restoration, such as a crown, to protect the tooth from fracturing.
- This final restoration is not included as part of your treatment at the Leeds Dental Institute and must be arranged separately with your general dentist.
- It is encouraged to discuss the timing and associated costs of the crown with your dentist in advance.
- Failure to have this done promptly significantly increases the risk of treatment failure or tooth fracture.
- The treated tooth is usually monitored with periodic X-rays to check healing, which can take six months to four years or longer.
Alternative treatment choices
You have other options to consider:
- No treatment: Risks include pain, swelling, infection, cyst formation, bone loss, and premature tooth loss, which can lead to drifting teeth, bite changes, an altered smile, and chewing difficulties.
- Waiting for more definitive symptoms.
- Extraction: If the tooth is extracted, replacement options include no replacement, dentures, bridges, or implants.
- Root-tip removal surgery (apicectomy): This may also be an option.
To contact us in an emergency
For any other queries please contact Restorative Reception.
If you live far from Leeds Dental Institute, we understand that traveling for every appointment can be difficult – especially in the case of an emergency or flare-up. That’s why we offer shared care with your general dental practitioner (GDP). This means that for urgent problems or unexpected flare-ups between your visits with us, it may be more convenient for you to see your local dentist. We’ll work together with your GDP to ensure you receive the appropriate care and that your treatment continues smoothly.