Leeds Children’s Hospital news
Our Charities
Leeds Children’s Hospital is supported by a number of amazing charities and we couldn’t do what we do without them.

Leeds Children's Hospital is one of the UK’s largest specialist children’s hospitals offering a wide range of treatments and care for children from birth to young adulthood and beyond. Children's A&E is located at Leeds General Infirmary.
Leeds Children’s Hospital is supported by a number of amazing charities and we couldn’t do what we do without them.
CQC for Leeds Children’s Hospital Read the latest report
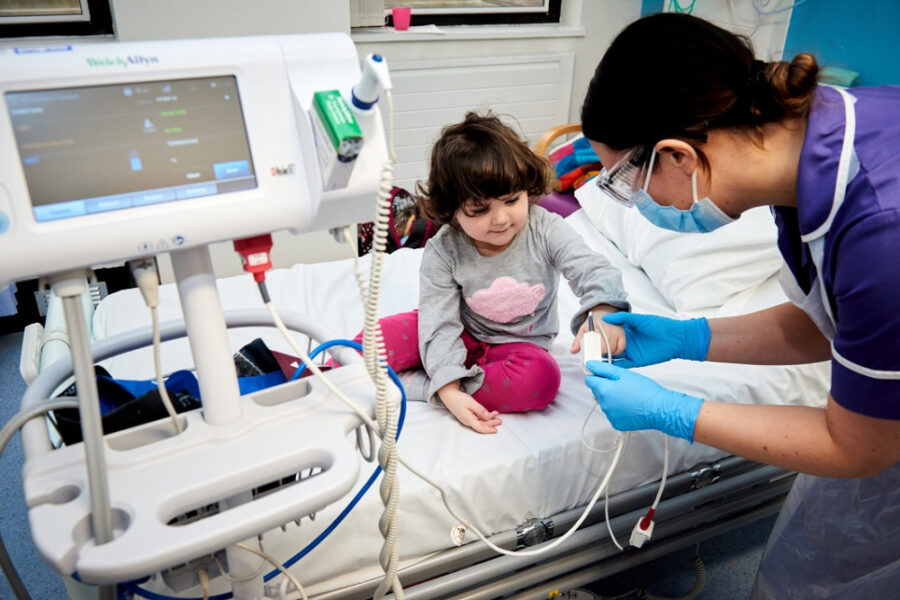
Children’s Clinical Research
Research is a priority at Leeds Children’s Hospital, and we aim to allow families the opportunity to take part in a wide variety of quality research, contributing to local, national and international studies

A new home for Leeds Children’s Hospital
For the first time in Leeds, we aim to bring children’s services together into one purpose-built state-of-the-art building designed around the needs of children and young people, their families and carers.

Careers at Leeds Children’s Hospital
Leeds Children’s Hospital is one of the UK’s largest children’s hospitals with state of the art facilities and treatments.